Home » Uncategorized
Category Archives: Uncategorized
A short talk on trauma and radical empathy
Without pretending to do justice to the vast research on “trauma,” it is variously defined as an event that threatens the person’s life and limb, making the individual feel he or she is going to die or be gravely injured (which would include rape). The blue roadside signs here in the USA that guide the ambulance to the “Trauma Center” (emergency department that has staff on call 7×24), suggest an emergency, usually but not always, a physical injury.
Cathy Caruth (1996) concisely defines trauma in terms of an experience that is registered but not experienced, a truth or reality that is not available to the survivor as a standard experience. The person (for example) was factually, objectively present when the head on collision occurred, but, even if the person has memories, and would acknowledge the event, paradoxically, the person does not presently experience it as something the person experienced in a way that a person standardly experienced the past event. The survivor experiences dissociated, repetitive nightmares, flashbacks, and depersonalization.

[Image credit (WIkimedia): Printmaker: Image: Prometheus being “traumatized” by the Vulture as punishment for giving the gift of fire to humanity (“mankind”): Cornelis Cortnaar Antwerp van: Titiaan (publisher of object), verlener van privilege: onbekend (vermeld op object)
Plate published: Rome
Date: 1566]
Strictly speaking, the challenge is not only that the would-be empathizer was not with the surviving Other when the survivor experienced the life-threatening trauma, but the survivor was physically present yet did not have the experience in such a way as to experience it. That may sound strange that the survivor did not experience the experience. Once again, one searches for words to capture an experience one did not experience. That is Caruth’s (1996) definition of “unclaimed” experience.
At the risk of oversimplification, Caruth’s work aligns with that of Bessel van der Kolk (2014). Van der Kolk emphasizes an account of trauma that redescribes in neuro-cognitive terms an event that gets registered in the body—burned into the neurons, so to speak, but remains sequestered—split off or quarantined— from the person’s everyday going on being and ordinary sense of self. The self is supposed to be a coherent unity—another example of a regulative idea—but a component of the self is split off due to a hypothetical, unknown traumatic cause. For both Caruth and van der Kolk, the survivor is suffering from an unintegrated experience of self-annihilating magnitude for which the treatment—whether working through, witnessing, or (note well) artistic engagement—consists in reintegrating that which was split off because it was simply too much to bear.
This artistic engagement with trauma has been described as “writing trauma,” for example, by Dominick LaCapra:
Trauma indicates a shattering break or caesura in experience which has belated effects. Writing trauma would be one of those telling after-effects in what I termed traumatic and post-traumatic writing (or signifying practice in general). It involves processes of acting out, working over, and to some extent working through in analyzing and ‘giving voice’ to [it] [. . . ]—processes of coming to terms with traumatic ‘experiences’, limit events, and their symptomatic effects that achieve articulation in different combinations and hybridized forms. Writing trauma is often seen in terms of enacting it, which may at times be equated with acting (or playing) it out in performative discourse or artistic practice (LaCapra 2001: 186–187).
Without intending to do so, LaCapra has unwittingly described Beloved (1987) (see Chapter 11), where the infant of the infanticide is literally reincarnated, reborn, in the person named “Beloved.” For LaCapra, working through such traumatic events is necessary for the survivors (and the entire community) in order to get their power back over their lives and open up the possibility of a future of flourishing. This “working through” is key for it excludes denial, repression, suppression, and, in contrast, advocates for positive inquiry into the possibility of transformation in the service of life. Yet the attempt at working through of the experiences, memories, nightmares, and consequences of such traumatic events often result in repetition, acting out, and, LaCapra’s key term, “empathic unsettlement.”
Such unsettlement is a challenge and an obstacle for the witness, therapist, or friend providing a gracious and generous listening. From a place of safety and security, the survivor has to do precisely that which she or he is least inclined to do—engage with the trauma, talk about it, try to integrate and overcome it. According to LaCapra, the empathic unsettlement points to the possibility that the vicarious experience of the trauma on the part of the witness leaves the witness unwilling to complete the working through, lest it “betray” the survivor, invalidate the survivor’s suffering or accomplishment in surviving.
Those traumatized by extreme events as well as those empathizing with them, may resist working through because of what might almost be termed a fidelity to trauma, a feeling that one must somehow keep faith with it” (LaCapra 2001: 22).
This “unsettlement” is a way that empathy breaks down, misfires, goes off the rails, resulting in empathic distress (Hoffman 2000). “Keeping faith with trauma” means the trauma itself has become an uncomfortable comfort zone. Extreme situations require extreme methods to engage and break up the emotional tangle.
Thus, according to Ruth Leys (2000), the traumatic events are “performed” in being written up as history or made the subject of a literary artwork. But the words, however authentic, true, or artistic, often seem inadequate, even fake. The “trauma” as brought forth as a distinction in language is ultimately inadequate to the pain and suffering that the survivor has endured, which “pain and suffering” are honored with the title of “the real” (as Kant might say). For Leys, the distinction “trauma” itself is inherently unstable oscillating between historical trauma—what really happened, which, however, is hard if not impossible to access accurately—and, paradoxically, literary language bearing witness by a failure of witnessing.
Moral trauma adds a challenging twist to what is traumatic about trauma. What is little recognized is that many survivors are also perpetrators (and vice versa). The survivor may also unwittingly (or even intentionally) become a perpetrator. The incarcerated prisoner of conscience steals a piece of bread from another prisoner, or to save his own life, falsely accuses another. One wants to say: This is tragic in the strict sense. Oedipus, Phaedra, Medea, practically the whole House of Atrius, are all both survivors and perpetrators.
Moral trauma is defined as the distressing emotional, behavioral, social, and sometimes spiritual aftermath of exposure to (including participation in) events in which a person’s moral boundaries are violated and in which individuals or groups are gravely injured, killed, or credible threat thereof is enacted (i.e., individuals are physically traumatized) (Litz et al 2009; see also Shay 2014). Examples of moral trauma include such things as being put in a situation where “I will kill you if you do not kill this person.” Generalizing on the latter example, the list includes morally fraught instances of double binds, valid military orders that result in unintentional harm to innocent people, situations in which survivors become perpetrators (and vice versa), soul murder (defined as killing the possibility of empathy and/or killing the possibility of possibility), and the Trolley Car Dilemma (Anonymous Wikipedia Content 2012, Foot 1967, Thomson 1976; see Chapter 11, Section: “The Trolley Car Dilemma and empathy”). In moral trauma people become both perpetrators and survivors, and such an outcome is characteristic of many (though not all) moral traumas.
Here radical empathy comes into its own. A person is asked to make a decision that no one should have to make. A person is asked to make a decision that no one is able to make—and yet the person makes the decision anyway, even if the person does nothing, because doing nothing is making a decision. A person is asked to make a decision that no one is entitled to make, which include most decisions about who should live or die (or be gravely injured). The result is moral trauma—the person is both a perpetrator and a survivor. Now empathize with that. No one said it would be easy.
Hence, the need for radical empathy. Extreme situations—that threaten death or dismemberment—call forth radical empathy. Standard empathy is challenged by extreme situations out of remote, hard-to-grasp experiences to become radical empathy.
The treatment or therapy consists of the survivor re-experiencing the trauma vicariously from a place of safety, an empathic space of acceptance and tolerance. In doing so the trauma starts losing its power and when it returns, it does so with less force, eventually becoming a distant unhappy and painful but not overwhelming memory.
For further reading, see van der Kolk 2014; LaCapra 2001; Leys 2000; Caruth 1995, 1996; Scarry 1985, Freud 1920.) See also Agosta (2025) Radical Empathy in the Context of Literature, Chapter 11, Sections: “The Trolley Car Dilemma and empathy” and “The four horsemen arrive.”
References
Lou Agosta. (2025). Radical Empathy in the Context of Literature, Chapter 11, Sections: “The Trolley Car Dilemma and empathy” and “The four horsemen arrive.” New York: Palgrave.
Anonymous Wikipedia Content. (2012). Trolley problem (The trolley dilemma). Wikipedia: https://en.wikipedia.org/wiki/Trolley_problem [checked 2023-06-25]
Cathy Caruth. (1996). Unclaimed Experience: Trauma, Narrative, and History. Baltimore: John Hopkins.
Philippa Foot. (1967). The problem of abortion and the doctrine of the double effect. Oxford Review, No. 5. In Foot, 1977/2002, Virtues and Vices and Other Essays in Moral Philosophy. Oxford: Oxford UP, 2002: 19–32. DOI:10.1093/0199252866.001.0001.
Sigmund Freud. (1920). Beyond the Pleasure Principle. The Standard Edition, Vol 18, New York and London: W.W. Norton: 1–64.
Martin L. Hoffman. (2000). Empathy and Moral Development: Implications for Caring and Justice. Cambridge, UK: Cambridge UP.
Dominick LaCapra. (2001). Writing History, Writing Trauma. Baltimore: John Hopkins.
Ruth Leys. (2000). Trauma: A Genealogy. Chicago: University of Chicago Press.
B. T. Litz et al Moral injury and moral repair in war veterans: a preliminary model and intervention strategy. Clin Psychol Rev. 2009 Dec;29(8):695-706. doi: 10.1016/j.cpr.2009.07.003. Epub 2009 Jul 29. PMID: 19683376.
Elaine Scarry. (1985). The Body in Pain: The Making and Unmaking of the World. Oxford: Oxford UP.
J. Shay, (2014). Moral injury. Psychoanalytic Psychology, 31(2), 182-191. https://doi.org/10.1037/a0036090
Judith Jarvis Thomson. (1976). Killing, letting die, and the trolley problem, The Monist, vol. 59: 204–217.
Bessel van der Kolk. (2014). The Body Keeps the Score. New York: Viking Press.
(c) Lou Agosta, PhD, and The Chicago Empathy Project
How I changed my relationship with pain
Expanded power over pain is a significant result that may usefully be embraced by all human beings who experience pain – which describes just about everyone at some time or another. Acute pain communicates an urgent need for intervention; chronic pain is demoralizing and potentially life changing. Intervention required!
People who do not experience standard amounts of pain are at risk of hurting themselves. Dr. James Cox, senior lecturer at the Wolfson Institute for Biomedical Research at University College London, notes, “Pain is an essential warning system to protect you from damaging and life-threatening events” (Jacquelyn Corley (Stat2019)). Admittedly not experiencing pain is a rare and concerning condition from which few of us suffer. Hence the practical approach considered here for the rest of humanity.
I changed my relationship to pain by working on the relationship. The result is that less pain occurs in my life and the pain that I do experience does not dominate my life. If one is completely pain-free, one is probably dead, which has different issues.
The following behaviors made a difference. Regular exercise, healthy diet, spiritual discipline (I have trained extensively in Tai Chi, but Yoga and/or meditation encompass the same results), consultations with professionals of one’s choice including medical doctors; and, here is the wild card, the purpose of this post: education in the different types of pain, including but not limited to acute pain versus chronic pain. The reader may say, “Holy cow! That’s too much work!” However, if the reader is in enough pain, then consider the possibility. What’s the alternative? Continue to suffer? Medically assisted suicide (where legal)? Opioids? The latter in particular have a place in hospice (end of life scenarios), in the week after surgery, but otherwise they are a deal with the devil. And, in any deal with the devil, be sure to read the fine print. “At a time when about 130 American die daily from opioid overdoses, scientists and drug companies are actively pursuing alternative non-opioid medications for acute and chronic pain” (Jacquelyn Corley (Stat 2019)).
An example will be useful. I changed my relationship to pain, following my MDs guidance, by taking a double dose of NSAIDs – non steroidal anti-inflammatory “pain killers”. The idea is to “kill” the pain without killing the patient. This is no joke because NSAIDs such as Aleve can damage the mucous membranes of the gastro intestinal track (e.g., stomach), leading to ulcer-like conditions and the accompanying risks (not detailed here), which is why, even though they are over-the-counter, consultation with a medical doctor is important.
Doing Tai Chi changed my relationship to pain. Your mileage may vary, but I started to see results after ten weeks of dedicated daily work. My Tai Chi training has continued with one lengthy interruption for six years. My experience was the practice moved the pain threshold up. That is, I did not experience pain as acutely and when I did experience pain, it did not bother me as much. This can be a double-edged consideration. For example, the Tai Chi exercise of “holding the ball” is a stress position. One really needs a picture to see what this is.
One stands there with one’s arms encompassing a large ball at about the level of one’s chest with one’s hips tucked slightly as if sitting back. One’s whole body is engaged and conditioned. After about ten minutes one starts to heat up and after about fifteen minutes one starts to sweat. This is Tai Chi, not Yoga, but Mircea Eliade discusses similar stress positions that generate Shamanic Heat (Eliade, (1964), Shamanism, translated Willard Trask. Princeton University Press (Bollingen)).
Now a word of caution regarding the pain threshold. I went for a dermatological treatment and I got burned, literally, (fortunately, not too seriously), because I did not say “Stop – it hurts!” Granted that most people want to experience less pain, it is important to not extinguish pain completely, because pain in its acute presentation is trying to tell one something – in this case, injury to one’s skin due to heat.
Here is another example. A colleague has an inflamed ankle. It throbs. It hurts. It is not fractured but imaging shows it is enflamed, stressed out. The thing is that this is not just the person’s sprained ankle – it is his whole life. Since he needs to lose weight, he needs to get exercise. Because he cannot get sufficient exercise, he cannot lose weight. The extra weight contributes to the ankle continuing to be stressed. Double-bind! Rock and the hard place. How is this individual going to break out of this tight loop? Now I know this is going to sound crazy, but here it is: Follow doctor’s orders! Go to the physical therapy! If you have got to wear “the boot” for a couple of weeks, do so. Start low (with the number of repetitions of exercises) – go slow. If the person had access to a swimming pool, that would be ideal, but that might not be workable for many people. SPA-like treatments, soaks in Epsom salts in sensory deprivation pods have value.
Many parallel examples can be cited in which a person knows exactly what she has to do (don’t even worry about the doctor) – why is the person not doing it? Many reasons exist, but one of them is that suffering becomes a comfort zone. Suffering is sticky. “Yes, I am miserable,” the individual says, but it is a familiar misery. Suffering has become an uncomfortable comfort zone. What would it take to give that up? Once one realizes, “This is what crazy looks like,” it becomes easier to give up the suffering. This is not a deep dive into the psychology of the unconscious, yet this is not merely a physical challenge. Yes, the ankle hurts – objectively, there is even an image that shows inflammation, albeit hazy and faint. However, even if there weren’t evidence of an injury – and soft tissue damage often escapes imaging, the emotional issue – ambivalence about one’s body image (“weight”) – gets entangled with the person’s whole life. In this case, a struggle with unhealthy excess weight – and the person’s emotions run with the ball – elaborate the injury psychologically. This is also a form of catastrophizing or awfulizing (made famous by cognitive behavioral therapy (CBT)), but CBT did not invent it.
I gave the example of an inflamed ankle, but it might also apply to lower back pain, headaches, asthma, irritable bowel syndrome (IBS), which are notoriously difficult to diagnose medically. Speaking personally, I want a quick fix. We all do. However, after a while, if the “fix” does not occur, there is no in principle limit on the amount of time and effort one can spend trying to find a quick fix. After a certain time, one gets a sense that one might put the time and effort into incremental progress – finding whatever moves the dial – whatever shifts the stuckness. Here’s what I did not want to hear: This is gonna take some work. After a time, one decides to roll up the sleeves and do the hard work need to get one’s power back. Healthy diet and a well-defined exercise program are important components. Finding an MD and/or health care provider including physical therapist where the interpersonal chemistry works is on the critical path to dialing down the suffering. Here “interpersonal chemistry” is another description for empathy. Look for someone whose empathy is open enough to encompass one’s pain and suffering without being coopted by it. This is the critical path to recovery.
The distinction between acute pain and chronic pain needs to be better understood by the average citizen. An excerpt from Neurology 101 may be useful. In acute pain, the peripheral nervous system in the body’s appendages such as one’s toes reports via neural connections to the central nervous system (e.g., the brain in one’s head). The impact of a heavy object such as a large brick with my toe releases neurotransmitters at the nociceptors (we are not talking Greek and “nocio” means “pain”). The mechanics are such that a message is delivered from the periphery to the center that what is in effect a boundary violation – an injury – has occurred. The brain then tells the toe to hurt – “Ouch!” The message is delivered seamlessly to the conscious person to whom the toe “belongs” in the neural map that associates the body with conscious experience unfolding in the person’s awareness. The toe which had quietly been doing its job in helping the person walk, balance, be mobile now makes a lot of “noise” – it starts throbbing. This is what acute pain feels like.
With chronic pain the scenario gets complicated. If the injury is subjected to other stressors, slow to heal, reinjured, or otherwise neglected, then the pain may continue across a period of days or weeks and become habitual. In effect, the pain signal becomes a bad habit. The pain takes on a life of its own. What does that even mean? What starts out as a way of reminding the person to attend to the injury gets stuck on “repeat”. Like the marketing company that keeps sending your notices even after you specify “Do not solicit!” The messaging is not just from the toe to the brain, from the periphery to the center, but it gets reversed. The messaging is from the center to the periphery, from the brain to the body part. The brain tells the periphery to hurt. Chronic pain becomes a source of suffering. Here “suffering” expands to include worry that anticipates and/or expects pain, which gets further reinforced when the pain actually shows up.
The poster child for chronic pain is phantom limb pain. Not all pains are created equal. Phantom limb pain provides compelling evidence that pain is “in one’s head” only in the sense that pain is in the brain and the brain is in one’s head. Only in that limited sense is pain in one’s head. Yet the pain is not imaginary. Documented as early as the American Civil War by Silas Weir Mitchell, individuals who had undergone amputation, felt the nonexistent, missing limb to itch or cramp or hurt. The individuals experienced the nonexistent tendons and muscles of the missing limb as cramping and even awakening the person from the most profound sleep due to pain (As noted, further in Haider Warraich. (2023). The Song of Our Scars: The Untold Story of Pain. New York: Basic Books, pp. 110 – 111).
Fast forward to modern times and Ron Melzack’s gate control theory of pain marshals such phantom limb pain as compelling evidence that the nervous system contains a map of the body and the body’s pains point, which map has not yet been updated to reflect the absence of the lost limb. In effect, the brain is telling the individual that his limb is hurting using an obsolete map of the body – the memory of pain. Thus, the pain is in one’s head, but not in the sense that the pain is unreal or merely imaginary. The pain is real – as real as the brain that is indeed in one’s head and signaling (“telling”) one that one is in pain. (R. Melzack, (1974), The Puzzle of Pain. Basic Books.)
Whatever the level of pain, stress is probably going to make it feel worse. Therefore, stress reduction methods such as meditation, Tai Chi, Yoga, time spent soaking in a sensory deprivation pod, and SPA-like stress reduction methods are going to be beneficial in moving the pain dial downward.
One question that has not even occurred to scientists is whether it is possible to have the functional equivalent of phantom limb pain, even though the person still has the limb functionally attached to the body. This sounds counter-intuitive, but think about it. If there is a map of the body’s pain points in the central nervous system (the brain), there is nothing that says “phantom” pains cannot occur even if an appendage still exists. For example, the high school football player who needs the football scholarship to go to college because he is weak academically; he is not good at baseball, but actually hates football. He incurs a soft tissue sports injury, which gets elaborated due to emotional conflict about his ambivalent relationship with football, leaving him on crutches for far-too-long and both physically and symbolically unable to move forward in his life. As if the only three life choices are football, baseball, and academics?! Note that the description of the injury “painful soft tissue” already opens and shuts approaches to treatment. That is the devilish thing – what is the actual and accurate description? Thus, due to the inherent delays in neuroplasticity – the update to the brain’s map of the body is not instantaneous and one does not have new experiences with a nonexistent limb – pain takes on a life of its own.
Though an oversimplification, the messaging between the peripheral and central nervous systems is reversed. Instead of the peripheral limb telling the brain of a “hurt,” the brain develops a “bad habit” of signaling pain and tells the limb to hurt. That is the experience of chronic pain – pain has a life of its own – pain becomes the dis-ease (literally), not the symptom. What then is the treatment, doctor? Physical therapy (PT) – exercises to strengthen the knee and, in effect, teach him to walk again.
Chronic pain is discouraging, demoralizing, fatiguing, exhausting, negatively impacting one’s mental status. I have been cagey about my own experience of pain in this post, but it is a matter of record that I have osteoarthritis, a progressive deterioration of the cartilage in joints such as occurs in people who are getting older and who are long term runners. The person understandably and properly continuously asks himself – what am I experiencing? And does it include pain? No one is saying the “cure” is don’t think about it (pain), don’t worry about it. No one is saying “play hurt”? “Playing hurt” is a bad idea for so many reasons, including one is going to make a bad injury worse. Professional athletes who “play hurt” may indeed get a bunch of money, but they also often dramatically shorten their careers – and that costs them money.
While distraction from one’s pain can be useful in the short term, it is not a sustainable solution. Rather when, after medical determination of the sources of pain are determined to be unable to be completely extinguished or eliminated, one is saying undertake an inquiry into what one is really experiencing. Rather than react to the uncomfortable twinges and twitches, bumps and thumps, prodding and pokes, that one encounters, ask what one is really feeling. Undertake an inquiry into what one is experiencing. If, upon consideration, the answer is “The pain is acute going from 4 to 8 to 9 on the 10 point scale,” then stop and call for backup, including taking pain killers such as NSAIDS as recommended by an MD.
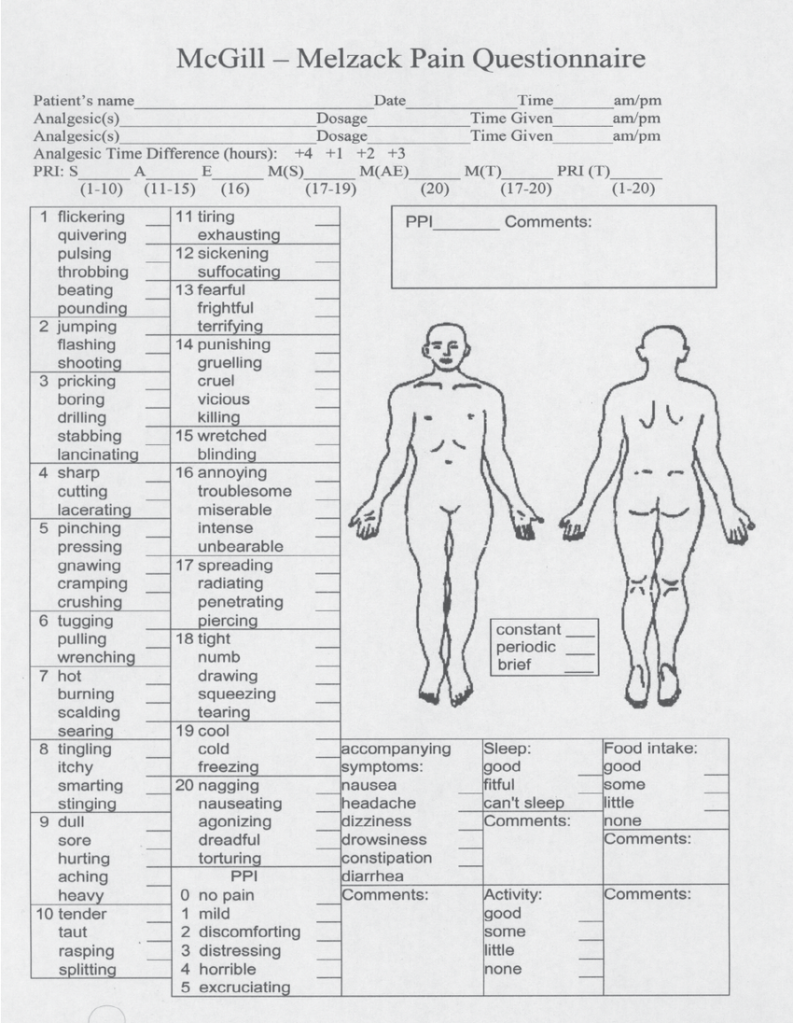
Here the vocabulary of pain is relevant. See Melzack’s McGill pain chart. [List the vocabulary]
Further background information will be useful. Haider Warraich, MD, in The Song of Our Scars: The Untold Story of Pain (Basic Books, 2023) radicalizes the issue of pain that takes on a life of its own before suggesting a solution. After providing a short history of opium and morphine and opioids, culminating “in the most prestigious medical school on earth, from the best teachers and physicians, we [medical students] were unknowingly taught meticulously designed lies” (p. 185), that is, prescribe opioids for chronic pain. The reader wonders, where do we go from here? To be sure opioids have a role in hospice care and the week after surgery, but one thing is for certain, the way forward does not consist in prescribing opioids for chronic pain.
After reviewing numerous approaches to integrated pain management extending from cognitive behavioral therapy and acceptance and commitment therapy (ACT) to valium, cannabis and Ketamine – and calling out hypnosis (hypnotherapy) as a greatly undervalued approach (no external chemicals are required, but the issue of susceptibility to hypnotic suggestibility is fraught) – Dr Warraich recovers from his own life changing back injury in a truly “physician heal thyself” moment thanks to dedicated PT, physical therapy (p. 238). If this seems stunningly anti-climactic, it is boring enough to have the ring of truth earned in the college of hard knocks, but it is a personal solution (and I do so like a happy ending!), not the resolution of the double bind in which the entire medical profession finds itself (pp. 188 – 189). The way forward for the community as a whole requires a different, though modest, proposal. The patient signs up for and completes physical therapy (PT), a custom set of exercises tailed to his pain condition and mobility issues.
The philosopher Ludwig Wittgenstein wrote, “The body is the best picture of the soul.” The default since René Descartes is to distinguish physical pain from psychic pain – what used to be called the difference between “body” and “soul” before science “proved” that the soul did not exist. (Once again, we are talking Greek “psyche” is the Greek word for “souI.”) Nevertheless, in spite of the “proof” that the soul does not exist, soul-like phenomena keep showing up. For example, if the person’s “soul” is regularly subjected to negative verbal feedback from those in authority, the person becomes physically ill – ulcers, headaches, lower back pain, irritable bowel syndrome (IBS). As noted, these are notoriously difficult to diagnoses. The adverse childhood experience survey (ACE) provides solid evidence that psychic and moral injuries correlate significantly with major medical disorders (e.g., Felitti 2002).
One big issue is that we (science and scientists) lack a coherent, effective account of emergent properties. One with neurons. The alternative is the current reductive paradigm according to which, in spite of contrary assertions, on has trouble explaining that things really are what they seem to be – that table are tables andmade of microscopic components such as atoms. We start with neurons. We are neurons “all the way down.” Neurons generate stimuli; stimuli generate sensations/experiences; experiences generate [are] responses; responses form patterns; patterns generate meaning; meaning generates language. With the emergence of language, things really start to get interesting. Organized life reaches “take off” speed. Language generates community; community generates – or rather is functionally equivalent to – culture, art, poetry, science, technology, and the world as we know it.
What about individuals who are put in a double-bind by circumstances as when someone in authority makes a seemingly impossible demand? For example, the army Sargent gives what seems to be a valid military order to the corporeal to shoot at the rapidly approaching auto, thinking it is a suicide car bomb, but it is really an innocent family. The soldier, thinking the order is valid and that he is protecting his team, follows the order. The solider is now both a perpetrator and a survivor. People have gotten hurt who ought not to have been hurt. Moral inquiry. Moral trauma has occurred. Tai Chi is not going to save this guy. This take the form of guilt – which is aggression – hostile feeling and anger – turned against one self. The individual’s agency – the individual’s power as an agent to choose – is compromised by contingent circumstance, including the individual’s unavoidable choice in the circumstance, since taking no action is also a choice.
This is why the ancient Greeks invented tragedy. A careful reading of the Greek tragedies, which cannot be adequately canvassed here, shows that virtually every tragic hero has the compromised agency characteristic of a double bind. Oedipus is a powerful agent, yet compromised and brought low by inadequate information. Information asymmetries! Antigone’s agency is bound, doubly, by the conflict between the imperatives of politics and the integrity of family. Agamemnon’s agency is compromised by the negative aspect of honor and pride and an overweening narcissism. Iphigenia’s agency is compromised by literally being bound and gagged (admittedly a limit case). Double-binds have also been hypothesized to contribute to the causation of major mental illness (Bateson 1956). Contradictory messages from parents, explicit versus implicit, spoken versus unspoken, are particularly challenging. Here the fan out to related issues is substantial.
I changed my relationship to pain and suffering by reading all thirty existing Greek tragedies. One might say if something is worth doing, it is worth over-doing, and the reader might try starting with just one. Examples of pain and suffering occur in abundance: acute pain – Hercules puts on the poisoned cloak, which burns his flesh; chronic pain – Philoctetes has a wound that will not heal and throbs periodically with painful sensations; and suffering – Oedipus is misinformed about who is his birth mother and after having children with her he suffers so from his awareness of his violation of family standards that he mutilates himself, tearing his eyes out. The latter would, of course, be acute pain, but the cause, the trigger, is thinking about what he has done in relation to the expectations of the community, namely, violating the incest taboo.
Now, according to Aristotle, the representation of such catastrophes is supposed to evoke pity and fear in the audience (viewer) of the classic theatrical spectacle. Indeed, such spectacles – even though the violence usually happens “off stage” and is reported – are not for the faint of heart. We seem to want to identify with the characters in a narrative, which, in turn, activates our openness to their experiences in an entry level empathy that communicates a vicarious experience of the character’s struggle and suffering. Advanced empathy also gets engaged in the form of appreciation of who is the character as a possibility in relation to which the viewer (audience) considers what is possible in her of his own life. One takes a walk in the other’s shoes, after having taken off one’s own. Other examples of similar experiences include why (some) people like to see horror movies. One does not run screaming from the theatre, but conventionally appreciates that the experience is a vicarious one – an “as if” or pretend experience. Likewise, with “tear jerker” style movies – one gets a “good cry,” which has the effect of an emotional purging or cleansing.
Now I am not a natural empath, and I have had to work at expanding my empathy. In contrast, the natural empath is predisposed, whether by biology or upbringing (or both), to take on the pain and suffering of the world. Not surprisingly this results in compassion fatigue and burn out. The person distances him- or herself from others and displays aspects of hard-heartedness, whereas they are actually kind and generous but unable to access these “better angles.” It should be noted that empathy opens one up to positive emotions, too – joy and high spirits and gratitude and satisfaction – but, predictably, the negative ones get a lot of attention.
“Suffering” is the kind of thing where what one thinks and feels does make a difference. Now no one is saying that Oedipus should have been casual about his transgressions – “blown it off” (so to speak); and the enactment does have a dramatic point – Oedipus finally begins to “see” into his blind spot as he loses his sight. Really it would be hard to know what to say. Still, the voice of reality would council alternatives – other ways are available of making amends – making reparations – perhaps more than two “Our Fathers” and two “Hail Marys” as penance – what about community service or fasting? “Suffering” is not just a conversation one has with oneself about future expectations. It is also a conversation one has with oneself about one’s own inadequacies and deficiencies (whether one is inadequate or not). For example, unkind words from another are hurtful. In such cases what kind of “pain” is the hurt? We get a clue from the process of trying to manage such a hurt. The process consists in setting boundaries, setting limits, not taking the words personally (even though inevitably we do). The hurt lives in language and so does the response. Therefore, in an alternative scenario, one takes the bad language in and turns it against oneself. One anticipates a negative outcome. One gets guilt (once again, regardless of whether one has does something wrong or not).
The coaching? If you are suffering from compassion fatigue, then dial down the compassion. This does not mean become hard-hearted or mean. Far from it. This means do not confuse a vicarious experience of pain and suffering with jumping head over heels into the trauma itself. What may usefully be appreciated is that practices such as empathy, compassion, altruism are not “on off” switches. They are not all or nothing. Skilled executioners of these practices are able to expand and contract their application to suit the circumstances. To be sure, that takes practice. The result is expanded power over vicariously shared pain and suffering. One gets power back and is able to assist the other in recovering their power too. (Further tips and techniques on how to change one’s thinking and expand one’s empathy are available in my Empathy: A Lazy Person’s Guide (with 24 full color illustrations by Alex Zonis), also available as an ebook.)
Before concluding, I remind the reader that “all the usual disclaimers.” This is a personal reflection. The only data is my own experience and bibliographical references that I found thought provoking. “Your mileage may vary.” If you are in pain (which, at another level and for many spiritual people, is one definition of the human condition) or if you are in the market for professional advice, start with your family doctor. If you do not have one, get one. Talk to a spiritual advisor of your own choice. Above all, “Don’t hurt yourself!” This is not to say that I am not a professional. I am. My PhD is in philosophy (UChicago) with a dissertation entitle Empathy and Interpretation. I have spent over 10K hours researching and working on empathy and how it makes a difference. So if you require expanded empathy, it makes sense to talk to me. A conversation for possibility about empathy can shift one’s relationship with pain.
Bibliography
Bateson, G., Jackson, D. D., Haley, J. & Weakland, J., 1956, Toward a theory of schizophrenia. Behavioral Science, Vol. 1, 251–264.
Corley, Jacquelyn. (2019). The Case of a Woman Who Feels Almost No Pain Leads Scientists to a New Gene Mutation. Scientific American. March 30, 2019. Reprinted with permission from STAT. https://www.scientificamerican.com/article/the-case-of-a-woman-who-feels-almost-no-pain-leads-scientists-to-a-new-gene-mutation/
Eliade, Mircea. (1964). Shamanism. Princeton University Press (Bollingen).
Felitti VJ. (2002). The Relation Between Adverse Childhood Experiences and Adult Health: Turning Gold into Lead. The Permanente Journal (Perm J). 2002 Winter;6(1):44-47. doi: 10.7812/TPP/02.994. PMID: 30313011; PMCID: PMC6220625.
Melzack, R. (1974). The Puzzle of Pain. New York: Basic Books.
(c) Lou Agosta, PhD and the Chicago Empathy Project
Paul Ricoeur, Philosopher of Empathy
This article on Paul Ricoeur, empathy, and the hermeneutics of suspicion in literature will be engaging to students of Ricoeur and empathy alike. One can download the PDF directly from the journal Etudes Ricœeurienne / Ricoeur Studies website: http://ricoeur.pitt.edu/ojs/ricoeur/article/view/628
The article is in English and an abstract is cited below at the bottom. If the above link does not work for any reason, then scroll to the bottom, where one can download the PDF within this blog post.
Meanwhile, I offer a recollection of my personal encounter with Professor Ricœur starting when I was a third year undergraduate at the UChicago. (This is an excerpt from a pending manuscript on empathy in the context of literature.)
By the time I was an undergraduate in my junior year in college, Paul Ricoeur had just arrived at the University of Chicago. Professor Ricoeur had attempted to play a conciliatory role in listening to and addressing student grievances in the face of entrenched method of lecturing by ex cathedra by mandarin professors at the Sorbonne, Paris, France, and related schools in the system. Though Ricoeur did not use the word “empathy” in his role as administrator at the University of Nanterre, he was attempting to play a role in conflict mediation, during the strike of student and workers in Paris in May 1968, a role in which empathy is famously on the critical path.

[Photo: Paul Ricoeur, circa 1970 upon his arrival at the University of Chicago, looking for all the world like the Hollywood icon, James Dean. University of Chicago News office: Detailed photo credit below.]
Ricœur’s intervention in the dynamics of academic politics and expanding the community of scholars the way he had done in setting up a kind of philosophy university in the German prisoner of war camp for his fellow French prisoners in 1941 did not work as well as he had hoped. Though it would not be fair to anyone (or to be taken out of context), the Germans (at that moment) were less violent than the striking French students and Peugeot workers in 1968. The French students threw tomatoes at Ricœur and called him a “old clown”; whereas the University of Chicago “threw” at him a prestigious named professorship. He liked the latter better. Ricœur’s courses were open to undergraduates who got permission, too, so I signed up for two of them – Hermeneutics and The Religious Philosophies of Kant / Hegel. Insert here a mind-bending blur of hundreds of pages of reading interspersed with dynamic and engaging presentations of the material. After the somewhat softball oral exams, for which he charitably gave me a pass, my head was spinning, and I needed to take a year off from school to regroup. I am not making this up. I worked as a parking lot attendant selling parking passes, which was an ideal job, since I could read a lot—you know, German-English facing pagination of two separate philosophical texts. This interruption also gave me time to go out for theatre to work on overcoming my painful social awkwardness and try and get a date with a girl. This “therapy” worked well enough, though, like most socially inept undergraduates, I had no skill at small talk and tended to utter what I had to say out of the blue and without creating any context. When I returned to school the next year to finish up, I proposed doing a bachelor’s thesis on Kant’s Refutation of Idealism, and I went into Professor Ricoeur’s office to make my proposal. Ricoeur was team teaching “Myth and Symbolism” with Mircea Eliade, and the “Imagination and Kant’s Third Critique” with Ted Cohen. Without any introductory remarks—I don’t think I even said my name—I presented the idea for my bachelor’s thesis. Without further chit-chit, raising one finger in the air for emphasis and smiling broadly, the first thing he said to me was: “An internal temporal flux implies an external spatial permanence.” With the benefit of 20-20 hindsight, I consider this a suitably empathic response, albeit an unconventional one. My paper eventually got published in the proceedings of the Acts of the 5th International Kant Congress. Fast forward a couple of years, comprehensive written exams in philosophy, and I proposed to write a PhD dissertation in philosophy on empathy [Einfühlung] and interpretation. Max Scheler’s Essence and Forms of Feelings of Sympathy [Wesen und Formen der Sympathiegefühl] contains significant material on empathy, and is (arguably) an early version of C. Daniel Batson’s collection of empathically-related phenomena. I was reading it with Professor Ricœur. Meanwhile, a psychoanalysis named Heinz Kohut, MD, like so many, a refugee from the Nazis, was innovating in empathy in the context of what was to become Self Psychology. I told one of the faculty at the Chicago Institute for Psychoanalysis who was a mentor to me (and a colleague of Kohut), Arnold Goldberg, MD, about Ricœur’s Freud and Philosophy. Whether at my instigation or on Dr Goldberg’s own initiative (Ricoeur really needed no introduction from me), Dr Goldberg introduced Professor Ricoeur to the editors at the Journal of the American Psychoanalytic Association (JAPA) and the result was Ricœur’s publication “The Question of Proof In Freud’s Psychoanalytic Writings” in JAPA August 1977 [Volume 25, Issue 4 6517702500404]. Using graduate students as a good occasion for a conversation to build relationships, we all then had dinner at the Casbah, a middle eastern restaurant on Diversey near Seminary Avenues in Chicago’s Old Town.
It always seemed to me that Professor Ricoeur was a teacher of incomparable empathy, though he rarely used the word, at least until I started working on my dissertation on the subject of empathy and interpretation. I am pleased, indeed honored, to be able to elaborate the case here, while also defending Ricœur’s hermeneutics of suspicion from a misunderstanding that has shadowed the term since Toril Moi’s discussion (2017) of it at the University of Chicago colloquium on the topic shortly before the pandemic, the details of which are recounted in the article.
ricouerempathyinthecontextofsuspicionDownload
ABSTRACT: This essay defends Paul Ricoeur’s hermeneutics of suspicion against Toril Moi’s debunking of it as a misguided interpretation of the practice of critical inquiry, and we relate the practice of a rigorous and critical empathy to the hermeneutics of suspicion. For Ricoeur, empathy would not be a mere psychological mechanism by which one subject transiently identifies with another, but the ontological presence of the self with the Other as a way of being —listening as a human action that is a fundamental way of being with the Other in which “hermeneutics can stand on the authority of the resources of past ontologies.” In a rational reconstruction of what a Ricoeur-friendly approach to empathy would entail, a logical space can be made for empathy to avoid the epistemological paradoxes of Husserl and the ethical enthusiasms of Levinas. How this reconstruction of empathy would apply to empathic understanding, empathic responsiveness, empathic interpretation, and empathic receptivity is elaborated from a Ricoeurian perspective.
Photo credit: University of Chicago Photographic Archive, [apf digital item number, e.g., apf12345], Hanna Holborn Gray Special Collections Research Center, University of Chicago Library.
This blog post and web site (c) Lou Agosta, PhD and the Chicago Empathy Project
The Empathy Diaries by Sherry Turkle (Reviewed)
Read the review as published in abbreviated form in the academic journal Psychoanalysis, Self, and Context: Click here
The short review: the title, The Empathy Diaries: A Memoir (Sherry Turkle New York: Penguin Press, 2021, 357 pp.) reveals that empathy lives, comes forth, in empathy’s breakdowns and failings. Empathy often emerges in clarifying a lack of empathy. This work might have been entitled, less elegantly, “The Lack of Empathy Diaries.” I found the book to be compellingly written, even a page-turner at times, highly recommended. But, caution, this is not a “soft ball” review.
As Tolstoy famously noted, all happy families are alike. What Tolstoy did not note was that many happy families are also unhappy ones. Figure that one out! Sherry’s answer to Tolstoy is her memoir about the breakthroughs and breakdowns of empathy in her family of origin and subsequent life.
Families have secrets, and one was imposed on the young Sherry. Sherry’s mother married Charles Zimmerman, which became her last name as Charles was the biological father. Within a noticeably short time, mom discovered a compelling reason to divorce Charles. The revelation of his “experiments” on the young Sherry form a suspenseful core to the narrative, more about this shortly.
Do not misunderstand me. Sherry Turkle’s mom (Harriet), Aunt Mildred, grand parents, and the extended Jewish family, growing up between Brooklyn and Rockaway, NY, were empathic enough. They were generous in their genteel poverty. They gloried in flirting with communism and emphasizing, in the USA, it is a federal offense to open anyone else’s mail. Privacy is one of the foundations of empathy – and democracy. Sherry’s folks talked back to the black and white TV, and struggled economically in the lower middle class, getting dressed up for Sabbath on High Holidays and shaking hands with the neighbors on the steps of the synagogue as if they could afford the seats, which they could not, then discretely disappearing.
Mom gets rid of Charles and within a year marries Milton Turkle, which becomes Sherry’s name at home and the name preferred by her Mom for purposes of forming a family. There’s some weirdness with this guy, too, which eventually emerges; but he is willing and a younger brother and sister show up apace.
In our own age of blended families, trial marriages, and common divorce, many readers are, like, “What’s the issue?” The issue is that in the late 1950s and early 1960s, even as the sexual revolution and first feminist wave were exploding on the scene, in many communities divorce was stigmatizing. Key term: stigma. Don’t talk about it. It is your dark secret. The rule for Sherry of tender age was “you are really a Turkle at home and at the local deli; but at school you are a Zimmerman.” Once again, while that may be a concern, what’s the big deal? The issue is: Sherry, you are not allowed to talk about it. It is a secret. Magical thinking thrives. To young Sherry’s mind, she is wondering if it comes out will she perhaps no longer be a part of the family – abandoned, expelled, exiled.
Even Sherry’s siblings do not find out about the “name of the father” (a Lacanian allusion) until adulthood. A well kept secret indeed. Your books from school, Sherry, which have “Zimmerman” written in them, must be kept in a special locked cupboard. How shall I put it delicately? Such grown up values and personal politics – and craziness – could get a kid of tender age off her game. This could get one confused or even a tad neurotic.
The details of how all these dynamics get worked out make for a page turner. Fast forward. Sherry finds a way to escape from this craziness through education. Sherry is smart. Very smart. Her traditionally inclined elders tell her, “Read!” They won’t let her do chores. “Read!” Reading is a practice that expands one’s empathy. This being the early 1960s, her folks make sure she does not learn how to type. No way she is going to the typing pool to become some professor’s typist. She is going to be the professor! This, too, is the kind of empathy on the part of her family unit, who recognized who she was, even amidst the impingements and perpetrations.
Speaking personally, I felt a special kinship with this young person, because something similar happened to me. I escaped from a difficult family situation through education, though all the details are different – and I had to do a bunch of chores, too!
The path is winding and labyrinthine; but that’s what happened. Sherry gets a good scholarship to Radcliffe (women were not yet allowed to register at Harvard). She meets and is mentored by celebrity sociologist David Riesman (The Lonely Crowd) and other less famous but equally inspiring teachers.
Turkle gets a grant to undertake a social psychological inquiry into the community of French psychoanalysis, an ethnographic study not of an indigenous tribe in Borneo, but a kind of tribe nonetheless in the vicinity of Paris, France. The notorious “bad boy” Jacques Lacan is disrupting all matters psychoanalytic. His innovations consist in fomenting rebellion in psychoanalytic thinking and in the community. “The name of the father” (Lacan’s idea about Oedipus) resonates with Turkle personally. Lacan speaks truth to [psychoanalytic] power, resulting in one schism after another in the structure of psychoanalytic institutes and societies.
Turkle intellectually dances around the hypocrisy, hidden in plain view, but ultimately calls it out: challenging authority is encouraged as long as the challenge is not directed at the charismatic leader, Lacan, himself. This is happening shortly after the students and workers form alliance in Paris May 1968, disrupting the values and authority of traditional bourgeois society. A Rashomon story indeed.
Turkle’s working knowledge of the French language makes rapid advances. Turkle, whose own psychoanalysis is performed by more conventional American analysts in the vicinity of Boston (see the book for further details), is befriended by Lacan. This is because Lacan wants her to write nice things about him. He is didactic, non enigmatic amid his enigmatic ciphers. Jacques is nice to her. I am telling you – you can’t make this stuff up. Turkle is perhaps the only – how shall I put it delicately – attractive woman academic that he does not try to seduce.
Lacan “gets it” – even amid his own flawed empathy – you don’t mess with this one. Yet Lacan’s trip to Boston – Harvard and MIT – ends in disaster. This has nothing – okay, little – to do with Turkle – though her colleagues are snarky. The reason? Simple: Lacan can’t stop being Lacan. Turkle’s long and deep history of having to live with the “Zimmerman / Turkle” name of the father lie, hidden in plain view, leaves Turkle vulnerable in matters of the heart. She meets and is swept off her feet by Seymour Papert, named-chair professor at MIT, an innovator in computing technology and child psychology, the collaborator with Marvin Minsky, and author of Mindstorms: Children, Computers and Powerful Ideas. Seymour ends up being easy to dislike in spite of his authentic personal charm, near manic enthusiasm, interestingness, and cognitive pyrotechnics.
Warning signs include the surprising ways Sherry have to find out about his grown up daughter and second wife, who is actually the first one. Sherry is vulnerable to being lied to. The final straw is Seymour’s cohabitating with a woman in Paris over the summer, by this time married to Sherry. Game over; likewise, the marriage. To everyone’s credit, they remain friends. Sherry’s academic career features penetrating and innovative inquiries into how smart phone, networked devices, and screens – especially screens – affect our attention and conversations.
Turkle’s research methods are powerful: she talks to people, notes what they say, and tries to understand their relationships with one another and with evocative objects, the latter not exactly Winnicott’s transitional objects, but perhaps close enough for purposes of a short review. The reader can imagine her technology mesmerized colleagues at MIT not being thrilled by her critique of the less than humanizing aspects of all these interruptions, eruptions, and corruptions of and to our attention and ability to be fully present with other human beings.
After a struggle, finding a diplomatic way of speaking truth to power, Turkle gets her tenured professorship, reversing an initial denial (something that rarely happens). The denouement is complete. The finalè is at hand.
Sherry hires a private detective and reestablishes contact with her biological father, Charles. His “experiments” on Sherry that caused her mother to end the marriage, indeed flee from it, turn out to be an extreme version of the “blank face” attachment exercises pioneered by Mary Main, Mary Ainsworth and colleagues, based on John Bowlby’s attachment theory. The key word here is: extreme.
I speculate that Charles was apparently also influenced by Harry Harlow’s “love studies” with rhesus monkeys, subjecting them to extreme maternal deprivation (and this is not in Turkle). It didn’t do the monkeys a lot of good, taking down their capacity to love, attachment, much less the ability to be empathic (a term noticeably missing from Harlow), leaving them, autistic, like emotional hulks, preferring clinging to surrogate cloth mothers to food. Not pretty.
In short, Sherry’s mother comes home unexpectedly to find Sherry (of tender age) crying her eyes out in distress, all alone, with Charles in the next room. Charles offers mom co-authorship of the article to be published, confirming that he really doesn’t get it. Game over; likewise, the marriage.
On a personal note, I was engaged by Turkle’s account of her time at the University of Chicago. Scene change. She is sitting there in lecture room Social Science 122, which I myself frequented. Bruno Bettelheim comes in, puts a straight back chair in the middle of the low stage, and delivers a stimulating lecture without notes, debating controversial questions with students, who were practicing speaking truth to power. It is a tad like batting practice – the student throws a fast ball, the Professor gives it a good whack. Whether the reply was a home run or a foul ball continues to be debated. I was in the same lecture, same Professor B, about two years later. Likewise with Professors Victor Turner, David Grene, and Saul Bellow of the Committee on Social Thought.
On a personal note, my own mentors were Paul Ricoeur (Philosophy and Divinity) and Stephen Toulmin, who joined the Committee and Philosophy shortly after Turkle returned to MIT. Full discourse: my dissertation on Empathy and Interpretation was in the philosophy department, but most of my friends were studying with the Committee, who organized the best parties. I never took Bellow’s class on the novel – my loss – because it was reported that he said it rotted his mind to read student term papers; and I took that to mean he did not read them. But perhaps Bellow actually read them, making the sacrifice. We will never know for certain.
One thing we do know for sure is that empathy is no rumor in the work of Sherry Turkle. Empathy lives in her contribution.
(c) Lou Agosta, PhD, and the Chicago Empathy Project
Empathy: Capitalist Tool (Part 3): Let’s do the numbers
Listen to this post on Spotify: https://open.spotify.com/show/6nngUdemxAnCd2B2wfw6Q6
Empathy by the numbers
I have been known to say: “We don’t need more data; we need expanded empathy.” But truth be told, we need both.
In an April/May survey by the human resources company Businessolver of some 1,740 employees, including 140 CEOs and some 100 Human Resources (HR) professionals, respondents reported:
37% of employees believe that empathy is highly valued by their organizations and is demonstrated in what they do.
Of the other 63% of employees, nearly one in three employees believe their organization does not care about employees (29%).
One in 3 believe profit is all that matters to their organization (31%).
Nearly one in two believe their organization places higher value on traits other than empathy (48%).
The evidence supports a conclusion that a significant deficit exists between experience and expectations relating to empathy. On a positive note, 46% of employees believe that empathy should start at the top. This opens the way for business leaders to articulate the value of expanding business results through empathy. The same survey indicates that the three most important behaviors for employers to demonstrate empathy include:
listening to customer needs and feedback (80%);
having ethical business practices (78%);
treating employees well, including being concerned about their physical and mental well-being (83%).
Three behaviors that demonstrate empathy according to the Americans Businessolver Survey:
listening more than talking (79%);
being patient (71%);
making time to talk to you one-on-one (62%).
The five behaviors that demonstrate empathy in conversation include:
verbally acknowledging that you are listening (e.g. saying, “I understand”) (76%);
maintaining eye contact (72%);
showing emotion (70%);
asking questions (62%);
making physical contact appropriate for the situation (i.e. shaking hands) (62%).
All this is well and good. But is it good for business? The survey reports that 42% of the survey respondents say they have refused to buy products from organizations that are not empathetic; 42% of Americans say they have chosen to buy products from organizations that are empathetic; 40% of Americans say that they have recommended the company to a friend or colleague. The answer to “Is empathy good for business?” is “Yes it is!”
“Corporate empathy” is not a contradiction in terms
This section is inspired by Belinda Parmar’s article “corporate empathy is not an oxymoron.”[i] Belinda Parmar is one of those hard to define, engaging persons who are up to something. She is founder of the consultancy The Empathy Business. She is an executive, a self-branded “Lady Geek,” public thinker, woman entrepreneur evangelist, and business leader.
According to Parmar, her consultancy’s corporate Empathy Index is loosely based on the work of the celebrated neuropsychologist Simon Baron-Cohen’s account of empathy.[ii] Parmar states in the newly revised 2016 Empathy Index, “empathy” is defined as understanding our emotional impact on others and responding appropriately. How does one map this to the four dimensional definition in Figure 1 (see p. 41 above)?
This captures what our multi-dimensional definition of empathy has called “empathic interpretation.” Parmar’s definition also calls out both the aspects of “understanding” and “responding,” which nicely correspond to empathic understanding and responsiveness, respectively, but misses empathic receptivity. Thus, three out of four. Not bad. How these get applied is a point for additional discussion.
Parmar and company’s Empathy Index aims at measuring a company’s success in creating an empathic culture on the job. This is not just a spiritual exercise. Parmar reports that the top 10 companies in the 2015 Empathy Index increased in value more than twice as much as the bottom 10, and generated 50% more earnings according to market capitalization.[iii] Now that I have your attention, a few more details.
The Empathy Index reportedly decomposes empathy into three broad categories including customer, employee, and social media. These contain further distinctions such as ethics, leadership, company culture, brand perception, public messaging in social media, CEO approval rating from staff, ratio of women on boards, accounting infractions and scandals. Over a million qualitative comments on Twitter, Glassdoor, and Survation were classified and assessed as part of the process of ranking the companies. Impressive. There is also a “fudge factor.”
The Empathy Index used a panel selected from the World Economic Forum’s Young Global leaders, who were asked to rate the surveyed companies’ morality. Note that Belinda Parmar was herself one of these leaders at some point, though presumably not for purposes of her own survey. Further conditions and qualifications apply. The company must be publicly traded and have a market capitalization of at least a billion dollars. The companies were predominately companies in the US and UK, a few Indian and no Chinese (due to difficulty getting the data). All the companies on the index had large numbers of end-user consumers (see “The Most Empathetic Companies,” 2016, Harvard Business Review for further details on the methodology). [iv]
Presumably the absence of steel mill, oil service, and aero-space-defense companies is not a reflection on their empathy, but simply indicates the boundaries of the survey. The 2015 index is widely available publicly and will not be repeated here. Suffice to say that the top three companies in 2015 were LinkedIn, Microsoft, and Audi. Google was at 7; Amazon, 21; Unilever, 38; Uber, 59; Proctor & Gamble, 62; IBM Corp, 89; Twitter, 93; and 98, 99, and 100 were British Telecom Group, Ryanair, and Carphone Warehouse, respectively. Interesting. My sense is that being on the list at all and relative ranking on the list in comparison with companies in a similar industry is more important than any absolute value or the numeric score as such, though the absence of a intensely consumer-product-oriented company such as Nestlé does give one pause. It is a deeply cynical statement, but an accurate one, that you know the pioneers by the arrows in their backs.
The truth of this otherwise politically incorrect observation is that innovators do not get the product or service perfect the first time out, and competitors are strongly incented to criticize and try to improve on the original breakthrough. Therefore, I acknowledge the value of the Empathy Index, and I acknowledge Belinda Parmar’s contribution. Empathy is no rumor in the work Parmar and her team is doing. Empathy lives in the work she and her team are doing.
How shall I put it delicately? The challenge is distinguishing empathy from ethics, niceness, generosity, compassion, altruism, social responsibility, carbon footprint, education of girls (and boys), and a host of prosocial properties. As this list indicates, lots of things correlate with empathy. Lots of things are inversely correlated with empathy. Empathy is the source of the ten thousand distinctions in business, including correlation with improved revenue, and meanwhile empathy gets lost in the blender.
The Empathy Index is a brilliant idea—and I am green with envy in that I did not implement it. In a deep sense, the only thing missing in my life is that my name is not “Belinda Parmar.”
Yet the reduction to absurdity of corporate empathy progresses apace with the Empathy Index as carbon footprint, reputation on social media, and CEO approval rating get included.
This index was designed prior to the revelation that social networking systems had become a platform for a foreign power (Russia) to publish exaggerated, controversial positions designed to ferment social conflict over race, economics, and extremist politics in the USA. Presumably further checks and balances are needed prior to accepting the reputations culled from such networks, unless one wants to include the approval rating of Russian trolls. Nothing wrong with approval ratings as such, but I struggle to connect the dots with empathy. Empathy is now a popularity contest to drive reputation and, well, popularity.
An alternative perspective on corporate empathy
I acknowledge the engaging and powerful work being done by Belinda Parmer and associates to expand empathy in the corporate jungle. The challenges of engaging with empathy as a property of the complex system called a “corporation” should not be underestimated. However, I propose to elaborate an alternative point of view regarding corporate empathy.
Corporations are supposed to be treated as individuals under law, which makes sense if one restricts the context to having a single point of responsibility for the consequences of the corporation’s actions.
Thus, for example, the accounting department cannot say, “It’s not our fault; marketing made promises we were unable to honor while manufacturing cooked the books behind our back.” That is not going to work as an excuse. Whoever did it, the corporation is responsible. However, empathy in a corporate context is not additive in this way.
The empathy of the corporation is not the sum of the empathy of all the individuals. It is true that a single individual who becomes known as “unempathic” has the potential to “zero out” the empathy of the entire organization; but for empathic purposes, “corporate empathy” is the integral of the seemingly uncountable possibilities, interpretations, and responses of leaders, workers, stake-holders, across all the functions in the organization.
For example, when IBM says “everyone sells,” IBM does not mean that the geek in the software laboratory has a sales quota. That would be absurd. IBM means precisely that the geek in the lab sells by writing software code so great that it causes customers actually to call up the account (sales) representative and ask for it by name. This puts me in mind of Arthur C. Clarke’s science fiction saying: “Any sufficiently advanced technology is indistinguishable from magic.” Likewise, with empathy: the customer may not directly experience the empathy of the geek in the back office, but the commitment, functionality, and teamwork “back there” is so over-the-top, that the sales person’s empathy with the customer is empowered in ways that seem magical.
In this alternative perspective, a corporation is an individual that positions itself on the continuum between “empathy in abundance” and “empathy is missing” by enacting four practices: (1) listening (2) relating as a possibility (3) talking the other person’s perspective (4) demonstrating all of these—listening, relating as a possibility, and walking in the other’s shoes—such that the other person (customer, employee, stake-holder, general public) is given back the person’s own experience in relating to the corporation in a way that the person recognizes as the person’s own.
It has been awhile since the mantra of empathic receptivity, understanding, interpretation and response has been reiterated, so the reader is hereby reminded to check on Figures 1 and 3 in the previous chapters for a review as needed (see pp. 41, 89). Empathy is not something “owned” by the executive suite, marketing, human resources, or sales, to the exclusion of other roles. Everyone practices empathy.
Stake-holders may include the general public, whose well-being and livelihoods are impacted by corporate practices (or lack thereof). For example, the general public was profoundly affected (and not just by the price of gasoline) by the failure of an off-shore oil well in 2010 that sent some 205.8 million gallons of crude oil pollution into the Gulf of Mexico.
It is never good news when one’s corporate break down becomes a major motion picture—in particular, a disaster movie such as Deep Water Horizon. Note also this implies that empathy is not a method of waging a popularity campaign on social media.
If the corporation is British Petroleum (BP), then the empathic response might well be an acknowledgment that your experience of us is: “The only thing more foul than our reputation is the pollution perpetrated on the coastlines of Louisiana, Alabama, Mississippi, and Florida and the lives and livelihoods of the millions of people who live there.” And BP has to do this even while defending itself in court against major legal actions where anything one says can and will be used against you.
What does it mean for a corporation to listen? Ultimately customers, employees, stake-holders must decide if a corporation has been listening by the way the company’s representatives respond. At the corporate level, empathic receptivity (listening) and empathic responsiveness are directly linked.
“Empathically” means respond in such a way that boundaries between persons are respected and respectfully crossed, agreements with the other person (or community) are honored, the other is treated with dignity, the other’s point of view is acknowledged, and the other is responded to in such a way that the other person would agree, even if grudgingly, that its perspective had been “gotten.”
People test whether others have been listening by examining and validating their responsiveness. Responsiveness includes the questions that they ask and the comments that they make in response. Most importantly it includes follow up and follow through actions.
Once again, breakdowns point the way to breakthroughs. A less dramatic example than Deep Water Horizon? From a customer perspective, here is an example of an everyday breakdown: “Corporations to customers: Stop Calling! Go to the web instead. Fill out the form, and wait for a response”—usually in an undefined time. The experience is one of being left hanging.
Today many corporations prefer that the customer interact with them through their web site, because web sites are less expensive than call centers. Phone numbers are disappearing from web sites; and even when a phone number is present, it may not be the proper one. The phone number at the bottom of a press release causes the phone to ring in the marketing department, not customer service.
Even when a phone number is available, the wait time is long and the service representative, who is a fine human being, is poorly informed. What is the experience? No one is listening. That is not a clearing for success in building an empathic relationship.
What then is? An ability to assess quickly what is the break down, suggest a resolution, and have a defined process of escalation to open an inquiry into the problem. The breakthrough is when the customer call is acknowledged and the equivalent of the help desk trouble-shooter calls the customer back at the number provided to the automated system with the solution or proposed action. The technology to do this has existed ever since the call center was invented, but until Apple thought of it, no one configured it to work from outbound call center to customer.
From an employee perspective, an employee will experience the corporation as listening if the person who sets his or her assignments (“supervisor”) is a listener. That means creating a context in which a conversation between two human beings, who are both physically present, can occur. Given that one person may report to someone in a different city, teleconferencing has a great future as does a periodic in-person visit.
However, if the one person is multi-tasking, working on email while supposedly having a conversation with the other person, that is not listening. Eliminate distractions. Set aside emails. If one is awaiting an urgent update regarding an authentic emergency, then it is best to call that out at the start of the conversation. “I might have to interrupt to take a call from Peoria, where the processing plant has an emergency.”
An “open door” policy can mean different things, but I take it to mean that “anyone can talk to anyone” and not have to feel threatened with retaliation. An “open door” is a metaphor for “listen” or “be empathic.”
If an employee is having trouble focusing on the job, something is troubling her or him, and the listener demonstrates empathy by asking a relevant question or providing guidance that brings the trouble into the conversation: “Say more about that” or “Help me understand” can work wonders. As soon as the employee believes that someone is really listening, out come the details needed to engage in problem solving.
If we are engaging with what might be described as employee “personal issues” such as the ongoing need to care for a disabled parent or child, substance abuse, mental illness, corporations realize that managers are not therapists. Smart corporations marshal external resources that operate confidential crisis phone lines and referral services. It is not entirely clear what “confidential” means here, since if the employee is missing most people notice it; but presumably such an absence does not directly feed into the employee review process. Such personal assistance centers are able to make referrals to providers of medical, mental health, or legal services. The benefit for the corporation is that employee stress and distraction are reduced. The employee is able to continue contributing productively as an employee. It is an all around win-win.
Yet the employee and his crisis are predictably going to show up in the manager’s office at the end of the business day before a holiday weekend. This is perhaps the ultimate test of the manager’s empathy. He or she is now being addressed as a fellow human being by another human, all-too-human, human being.
This is an empathy test if there ever was one; and this is where practice and training can prepare the manager to respond appropriately by marshaling resources on short notice. In a crisis on Friday afternoon at 4 pm before a holiday weekend, managers can create loyalty for life in the commitment of the employee, who was assisted in a way that made a profound difference. “Above and beyond” recognition awards for the empathically responding manager are appropriate too.
Let us shift gears and take the conversation about corporate empathy up a level with a particular example. Nestlé has a portfolio of popular and even beloved brands that literally come tumbling out of the consumer’s pantry and refrigerator when one opens the door. Some 97% of US households purchase a Nestlé product, which extend from chocolate to beverages to prepared foods to baby food to frozen treats to pet products and beyond. You might not even know it, but Perrier, Lean Cuisine, Gerber, and Häagen Dazs are Nestlé brands. So are Purina pet products..
Nestlé is so committed to sustainability in nutrition, health, and wellness that it produces a separate annual report dedicated to identifying, measuring, and reporting on its progress against literally dozens of sustainability goals. After reviewing this material, as I did, the reader can hardly imagine that Nestlé has any commitments other than social responsibility, though Nestlé is a for profit enterprise and doing very well as one.
Sometimes our strengths are also our weaknesses. Nestlé is a strong contender to be the most empathic corporation on the planet, regardless of how one chooses to define empathy. Yet it did not even get on Belinda Parmar’s Empathy Index. What gives? A single blind spot in the 1970s, in which Nestlé leadership thought it saw a long term growth opportunity in infant (baby) formula, got in the way. Given the population growth in parts of Asia and Africa, Nestlé thought it could steal a march on the competition.
Nestlé had been a force in infant formula, especially for those babies whose mothers are unable to nurse due to illness or when it comes time to wean the infant. Yet it looks like corporate planners projected first world infrastructure onto the third world in an apparent breakdown in empathic understanding and interpretation. A world of good work and good will was destroyed or at least put at extreme risk.
Nestlé’s marketing of baby formula has created an enduring controversy. Starting in the 1970s Nestlé has been the target of a boycott based on the way that Nestlé marketed baby formula in the developing world.[i] From a public relations perspective, it has been a breakdown, if not a train wreck. The initial issue was supposedly that Nestlé was too aggressive in marketing baby formulation as a substitute for breast feeding. However, when one looks at the details, the issue really seems to be empathizing with the practice of breast feeding, given life in many third world countries. A breakdown in empathy?
The third world often lacks clean water, reliable power for sterilization of baby bottles, instruction labels in local languages that can be read and understood and followed by possibly illiterate or partially literate mothers. If the mother is healthy and lactating, breast feeding is a strong candidate to be the preferred method of infant feeding.
I have been known to say: “We don’t need more data, we need expanded empathy.” But, truth be told, both are required here.
Infant morbidity and mortality is reportedly three to six times greater for those infants using formula than for those who are breast fed.[ii]Nestlé responds—with a stance whose empathy is questionable—with a defensive conversation about compliance. Nestlé states that it fully complies with the 34th World Health Assembly code for marketing infant formula.
Nestlé’s Annual Review 2016 states with expanded empathy:
We support and promote breastfeeding as it is the best start a baby can have in life. In cases when breastfeeding is not possible due to medical or physical conditions, infant formula is the only breast-milk substitute recognised by the World Health Organisation. Nestlé Nutrition provides high-quality, innovative, science-proven nutrition for mothers and infants to help them start healthy and stay healthy during the critical first 1000 days.[iii]
But the matter is complex. IBFAN (the International Baby Formula Action Network) states that Nestlé distributes free formula in hospitals and maternity wards in the third world. This seems literally like manna from heaven; but the free formula lasts only long enough for lactation to stop (“lactation,” of course, being the naturally occurring production of breast milk after the woman gives birth).
After leaving the hospital, the formula is no longer free, but because lactation has ceased, the family must buy the formula. Gotcha?! IBFAN also asserts that Nestlé uses “humanitarian aid” to jump start markets and does not label its products in the language spoken in the country where the product is sold. “Humanitarian aid” is not marketing, but then again maybe such “aid” has similar, if unintended, consequences as “free samples” in marketing. Further, IBFAN asserts that Nestlé offers gifts and sponsorship to influence health workers to promote its products.
Nestlé denies these allegations, and states that it is responsive, and ongoing steps are being taken to remedy the situation.[iv] Never was it truer that empathic interpretation is a dynamic process.
One person’s empathic responsibility is another person’s unempathic irresponsibility. Note that the duck-rabbit (see Figure 4, cited above, p. 182) maps to a single continuous line on the page. It is the “objective” reality of the line itself that starts resonating, flipping back and forth, when it encounters the human perception system. Perhaps it was just too complicated and controversial to include Nestlé in the Empathy Index, formulated by Belinda Parmer’s process.
Any corporation that commits to practicing empathy will find its commitment challenged in ways that an Empathy Index (as currently defined) cannot imagine—or capture.
So popularity contests are likely to remain the preferred method of expanding empathy in marketing departments, especially among those who are—you guessed it—popular! The easy way out? Among those who decide to do the tough work of empathy, acknowledging inauthenticities and cleaning up integrity outages, a corporation can practice empathy at a high level and also have a reputation that is (in)distinguishable from the tar-like asphalt that randomly washes up on the beach after an oil spill.
Empathy in the corporate environment is “trending,” but remains a work-in-progress with many trade-offs and opportunities for debate. Still, the battle is joined.
The challenge is to see the empathic forest for the trees. Corporate empathy means many things. In corporate speak, “empathy” becomes a synonym for “employee benefits,” “social responsibility,” “executive ethics,” “favorable feedback from employees,” and “team building.” For example, input to Parmar’s Empathy Index includes “carbon footprint,” “number of women on the Board,” and reputation on social networking media. Carbon footprint?
Connecting the dots between empathy and carbon footprint is definitely a work-in-progress.
Follow the money. Definitely. But do not follow it off a cliff.
Stake-holders—people who buy stocks or bonds in a publically traded company—give money to the company. They want money back in turn—cash flow or profit or both. Don’t tell me about empathy; show me the money!
Although some investors are interested in social responsibility, most investors are interested in profit. They are not asking for empathy or even particularly interested in empathy, unless they decide it can make money for them. As Chris Janson, country western, singer says: “They say money can’t buy happiness. [Pause.] But it can buy me a boat—and a truck to pull it.” Funny. The suspicion is that the good ol’ boy doesn’t get enough empathy from the supervisor down at the saw mill, and needs to get away to go fishin’, which, in turn, simulates an experience like stress reduction, a major result of empathy.
Saying that the purpose of business is to make money is like saying the purpose of life is to breathe. Keep breathing—and make money—by all means. But the purpose of life is to find satisfaction in one’s work, raise a family, write the great American novel (it’s good work if you can get it!), experience one’s efforts as contributing to the community and making a difference.
Likewise with business. Business is about delivering human value and satisfying human demands and goals, whether nutrition, housing, transportation, communication, waste disposal, health, risk management, education, entertainment, and so on. Even luxury and conspicuous consumption are human values, which show up as market demands.
The customer with a complaint is an example of supply and demand. The customer is “demanding” a product or service that satisfies the real or implied service level agreement. What is often not appreciated is that the customer is also often demanding empathy as part of the service level agreement.
Which direction is the empathy travelling? From employee to customer? From supervisor to employee? From executive to stake-holder? The one who gets paid the money provides the empathy along with the produce or service. Even fairly abstract financial instruments such as insurance and hedging future prices in commodities such as wheat or oil have a valid function in risk management and so have an empathic core of managing hope and fear about the future. The one exception I can think of? Trading derivatives and derivatives of derivatives becomes a formal financial form of gambling. Absent empathy, some people find that gambling provides them with the stimulation they require to feel alive.
One may argue that transportation does not require a Lamborghini and that a Honda Civic will do quite well, thank you; but the debate is still about the experience of brand equity, which is a proxy for empathy like “carbon footprint.” The purpose is to create satisfied customers, suppliers, buyers, sellers, and partners. Review the above-cited quote from Jack Welch that “shareholder value is a result, not a strategy” (see p. 274 above). If one does these things well, addressing a demand in the market, the money shows up.
In conclusion, business people “get it”—empathy is good for business. Profit is a result of business strategy, implementation, and operations, not “the why” that motivates commercial enterprise. And if profit shows up that way (as the “the why”), then you can be sure that, with the possible exception of index derivative hedging, it is a caricature of business and a limiting factor. Business prospers or fails based on its value chain and commitment to delivering value for clients and consumers. However, as noted, some of the things that make people good at business make people relatively poor empathizers.
Business leaders lose contact with what clients and consumers are experiencing as the leaders get entangled in solving legal issues, reacting to the competition, or implementing the technologies required to sustain operations. Yet empathy is never needed more than when it seems there is no time or place for it. This is a challenge to be engaged and overcome.
What to do about it? Practice expanded empathy. Empathy is on the critical path to serving customers, segmenting markets, positioning products (and substitutes), psyching out the competition—not exactly empathy but close enough?—building teams and being a leader who actually has followers. Empathy makes the difference for contributors to the enterprise at all levels between banging on a rock with a hammer and building a cathedral. The motions are the same. When the application of empathy exposes and strengthens the foundation of community, then expanding empathy becomes synonymous with expanding the business.
Building customer communities, building stakeholder communities, building teams that work, are the basis for product innovation, brand loyalty, employee commitment, satisfied service level agreements, and sustained or growing market share. Can revenue be far behind? Sometimes leaders don’t need more data, leaders need expanded empathy, though ultimately both are on the path to satisfied buyers, employees, and stakeholders. If the product or service is wrappered in empathy, has an empathic component as part of the service level agreement, gets traction in the market, and beats the competition’s less empathic offering, then we have the ultimate validation of empathy. We do not just have empathy. We have empathy, capitalist tool.
[i] Belinda Parmar. (2016). Corporate empathy is not an oxymoron, Harvard Business Review: https://hbr.org/2015/01/corporate-empathy-is-not-an-oxymoron [checked on June 30, 2017]. This article includes the complete list of 100 companies.
[ii] Simon Baron-Cohen. (2011). The Science of Evil: On Empathy and the Origins of Cruelty. New York: Basic Books (Perseus).
[iii] Belinda Parmar. (2016). The most empathetic companies. 2016. Harvard Business Review, 12/20/2016: https://hbr.org/2016/12/the-most-and-least-empathetic-companies-2016 [checked on June 30, 2017].
[iv] Parmar 2016.
[i] Anonymous Contributors. (nd). Nestlé boycott, Wikipedia: https://en.wikipedia.org/wiki/Nestlé_boycott [checked on August 15, 2017].
[ii] Ibid., Nestlé boycott, Wikipedia
[iii] Nestlé Annual Review 2016: https://www.nestle.com/asset-library/documents/library/documents/an nual_reports/2016-annual-review-en.pdf: 20 [checked on 12/11/2017]. Note that Nestlé produces three (3) corporate annual reports every year. One for Nestlé International; one for Nestlé USA; and a third on Nestlé’s measurable commitments to social responsibility.
[iv] Op. cit.: Nestlé boycott, Wikipedia.
(c) Lou Agosta, PhD and the Chicago Empathy Project
Empathy and Literature: Transcript of Grand Rounds Talk (Oct 13, 2016)
This is a transcript of the talk.
The recommendation? Listen to the podcast: https://anchor.fm/lou-agosta-phd/episodes/Empathy-and-LIterature-Grand-Rounds-Presentation-at-Rush-Medical-University-October-13–2016-e177nvv
or watch the Youtube video: https://youtu.be/sYJvplP5cKo
Howard Kravitz, MD: Welcome to the partner psychiatry gran realms this morning is my pleasure to introduce the speaker dr. Lou Agosta got his PhD in philosophy at the University of Chicago with a dissertation entitled empathy and interpretation and running with that as his career scholarly activity ever since he’s an assistant professor of psychology at the Illinois School of Professional Psychology and Argosy University and instructor of philosophy at the University to call the Graham School of adult education and director of research at other gang psychotherapy services in Chicago he also as a psychotherapy practice in the Chicago community who specializes in making empathy present in his storytelling and listening – he’s committed to a gracious and generous listening based on empathy which I personally experienced a meeting with him this summer to talk about his idea for Grand Rounds – as an educator he teaches empathy in the history of and systems of psychology program at the Illinois School of Professional Psychology and Argosy University – he has published three scholarly academic books on empathy entitled – empathy in the context of philosophy – a rumor of empathy: rewriting empathy in the context of philosophy – and a rumor of empathy: narrative and recovery – he also undertook training as a psychodynamic therapist at the Chicago Institute for Psychoanalysis – however did not complete the program when he was summarily dismissed for asking publicly “is anyone beside me aware of a lack of empathy?” – so with that I will turn the program over to him
Lou Agosta [LA]: Well thank you so much dr. Kravitz for that introduction – so the challenge is to make empathy present – will we be able to do that in the next 45 or 50 minutes? I begin by acknowledging your empathy – you all are going to be doing some listening and I appreciate that and recognize that and acknowledge it – and I want to be concise and allow time for questions in interaction at the back end – some logistics and housekeeping make sure you have the color handout – if you don’t it’s in the back on the left side – there it says how empathy functions – 2-sided copying ladies and gentlemen – and then how empathy breaks down – so sometimes we can create a breakthrough based on a break down – and one of the results of the conversation that we’re going to have today among others is a short history of the distinction empathy – in fact the secret underground history of empathy – we’re going to define empathy –
Lou Agosta [LA]: we’re going to look at some examples of empathy through literature – so rather than clinical examples I’m going to ask you to take it up a level – the guidance is and with all due respect don’t be too concrete don’t be too literal let’s get our metaphorical transference thinking caps on and look at empathy of [in] some examples of world literature and then I’m going to make time – I’m going to say a few things about how empathy is teachable trainable – in fact that’s so important i am going to give you the answer right up front – basically people are naturally empathic – if we remove the obstacles to empathy, then empathy shows up – in other words, the obstacles to empathy are the such things as: denial, resistance, cynicism, bullying, aggression, bad language –
LA: I have a great Dilbert cartoon here -[make sure you] don’t get inside of a Dilbert cartoon – [it is] hilariously funny – closely related to empathy – [drive out] denial, cynicism, guilt, shame, and the like – remove the obstacles to empathy and it [empathy] naturally comes forth – so that’s the answer – what’s the question? – how do we train everyone ? – so we’re gonna circle around and return to this at the back end – we’re going to begin with a short secret underground history of empathy – so this is going to be blazingly concise –
LA: this is the part which you may find somewhat academic [but important] and there as you look at it in the upper left hand corner a man named David Hume [ who published] A treatise of human nature 1739 – [in the year] 1739 the word empathy in the English language was not even invented [it was not invented] until 1895 when a Cornell University psychologist – a man named Edward Bradford Titchenner was translating some of the works of Vilhelm Vundt [Wilhem Wundt] – I have to get my best German accent on there – it comes across as empathy – he [Titchener] makes up the word [empathy] – okay – meanwhile […] that’s why we have a secret underground history of empathy – Hume is writing and has at least five different definitions of sympathy – I say close enough – you have the hand out – the complete deck is on the URL on the lower left hand corner [see the youtube video for the slides] – I’m not going to speak slowly enough for you to take notes –
I’m going to tell you what the five different definitions of sympathy – they’re there and you can go back and get them – he never a stickler for consistency – the philosopher Hume divides sympathy as (1) emotional contagion – he defines sympathy as (2) suggestibility – the power of suggestion – (3) he defines it in a somewhat technical way as a double representation of a vicarious experience of another person combined with the idea of the other that matches closely to a modern definition of empathy that we find in psychology (4) he also defines sympathy as a delicacy of sympathy and taste and this matter of substituting a certain kind of sympathy in the experience of the work of art – this is the secret underground history of empathy – we relate to other people on a good day as if they were works of art – that is without use value – without manipulation – without knowing something – without categories – without argument – and [on] a less good day we struggle like everybody else – and finally as (5) benevolence – he defines sympathy as compassion or benevolence –
LA: and so we’ve got all these definitions – what the heck is it [empathy] – what is this definition so I sent the class [I was teaching at the time] out [to do research by asking people on the street] – I have everybody in the class – several classes – each student asked five people what they think empathy is – not members of your family people – you know moderately well – not really close – you know – but people you might work with or run across at the club or at the gym or something – so there’s a trend – so sometimes I go around saying we don’t need more Data we need expanded empathy – I’ve been known to say that – and nevertheless we need both data and empathy […] -I say more empathy – it’s like there’s something missing rather than something wrong – let’s expand – the languaging is significant as well – this is in the realm of tips and techniques- okay – so anyway – so the people go out and ask them and so here’s the trend: most people think empathy is something like compassion – they tell the story about altruism – they tell a story about charity – they tell the story about doing good – they tell the story about making difference – they tell a story about being nice and heavens knows ladies and gentlemen, the world needs more niceness – [yet niceness] it is distinct from empathy – we’re going to say a little bit more about that but first I want to very concisely touch on – as you look at the picture in the upper right hand corner – Immanuel Kant – he died in 1804 – he had the distinction between putting oneself in the position of the other person – he said enlarged thinking – think as the other [people] think and feel – so that’s top down – in effect we take that as the folk psychology definition of empathy – we take a walk in the other person’s shoes – where does the shoe pinch – where does the moccasin chafe – and then he also he once again interestingly and controversial enough in the context of a theory of art and beautiful nature he talks about the communicability of feeling – art is impossible without the communicability of affect – feeling – that’s stage one of empathy – now if you stop, [then] there you get emotional contagion – you get suggestibility – you get a certain kind of shared mutual enthusiasm – and there’s nothing wrong with that if there’s further processing upstream and downstream that’s going to occur – nevertheless it’s right there and then [we are going] around the circle –
LA: and this is why this is the secret underground history: on the bottom left – a man named Theodore Lipps – remember the movie Amadeus ?where you know Mozart is slaving away and the most famous man of his day a musician named is Antonio Salieri who today except for the movie Amadeus nobody would have ever heard of Antonio Salieri – I mean he’s not played – or they’ll give attention occasionally now because of the movie – right – and today Mozart – everybody knows Mozart’s music is played widely and nobody’s ever heard of Salieri until you come across the movie – well Lipps is Salieri to Freud’s Mozart – Lipps wrote several volumes in which he gives currency in the German language to the word Einfühlung [empathy] – he [Lipps] in effect replaces the distinction aesthetic taste judgment of a feeling of pleasure or displeasure with Einfühlung [empathy] – and he [Lipps] is significant because seven volumes of Lipps work are in the Freud Library – Freud encountered empathy by reading Theodore Lipps –
and [Freud] footnotes Lipps explicitly in Freud’s works on jokes and the relation to the unconscious – and the number of his aesthetic works – so moving right along there are twenty-two mentions of empathy in 24 volumes of the Freud Library as Harry Trosman MD and Simmons – our colleagues over at the analytic Institute – have done the scholarly work – here’s the point – almost every one of them [references to empathy] is mistranslated – freud says in so many words in his 1913 [year published] recommendations for physicians beginning psycho analytic treatment: you will go wrong if you begin with any other method besides empathy – quote end quote – it’s there and that gets mistranslated as sympathetic understanding – the Strachies [translators] will have a few other devaluing things to say about the word empathy so that’s the secret […] – the rest is history which we’re not going to do in the necessary detail – we’re going to move right along –
so most people think that empathy is compassion – and heavens knows the world needs more compassion – yet [compassion] it is not empathy – so what then is it ? Well basically we’re gonna have about two or three different definitions but the main definition which you have in front of you is to the effect – I know what the other person is experiencing because I experienced it also – not as a merger but as a vicarious experience – note vicarious experience contains the word Vicar which means representative – the etymology right as it actually works in this case if that is the the bishops representative to the community – the Vicar of something or other – and in any case combined with the distinction Other – and so basically here’s the distinction – empathy tells me what the other person is experiencing – and my good upbringing, my morals, my values, tell me what to do about it – and so that’s the compassion part – it’s in and its distinct – so having said that now here’s the most controversial slide I want you to pick up on this because it could be a controversial –
and I want – to quote to Jodi Halpern and I’m gonna wave Jodi’s book at you [entitled From detached concern to empathy: humanizing medical practice – Jodi Halperin – this is [published] 2001 so this has been around for a while and you know if we’re gonna have lunch afterwards – if you want to take a picture of the cover – I’ll bring it [the book] along with me and you can check it out but basically she says – the field of medicine empathy is a mode of understanding that specifically involves emotional resonance so it’s not just top down – it’s also bottom up – I’m getting some kind of a vicarious experience – this may or may not be the case – this may or may not be the case […] and so you know nevertheless she puts a stake in the ground and she is actually a psychiatrist – she has some stories
and I turn now to the explicit definition of empathy which we’re going to work with here and there are four phases to it – and that’s the handout – […] you get the handout – it’s on the left there – in the back table – so you want to be on the side: how empathy functions – […] so we’re gonna go around in a circle – we’re gonna go around in the circle here that would be actually counterclockwise – I’m open to the other person – I’m receptive – I have mirror neurons – and here’s where one can insert the underlying physiology – the underlying neurology – that’s not visible – here us mammals – we seem to resonate together – something is going on – we’re attached – it’s a myth that we aren’t related – we are related – physiologic\ally, biologicall,y and so [that is] phase one […]
phase two that creates a potential space for interaction – what’s possible in the relationship – do I relate to the other person as a means or end – do I relate to the other person as a possibility as a potentiality – we’re going to see an example of that and then actually you have to jump across so that gives us empathic receptivity- empathic understanding and empathic interpretation is the third aspect of empathy and that is the folk psychology of empathy – I take a walk in the other person’s shoes – I imaginatively change places with you – now that’s easier said than done because I don’t know you and nine times out of ten if I don’t, [then] I’m going to attribute to you aspects of my own character traits – Who I am – what I’m up to and that’s the challenge – right? – that’s not going to be and it’s going to be a psychological mechanism called projection which has its uses and is of interest – nevertheless is once again not empathy – and so get a view from over there but that does especially when I come up short I don’t know who you are – where you came from – then I go to the cognitive imaginative projection – and that’s very useful – and finally empathy can be a tree that falls in the forest without anybody being there – does it make a sound? does it make a difference? I have to say something I have to do something – a gesture- an aspect of behavior to let the other person know whether or not I have gotten what their experience is and sometimes that’s called empathic listening – that’ll work – good gracious listening – that maybe it is self sufficient but sometimes it’s not especially if I don’t know the other person – it may we’re highly verbal – you know there’s a lot of words and sometimes it’s necessary for me and so empathic responsiveness – so we’ve got receptivity – understanding – interpretation – and responsiveness –
I take the other person’s experience and give it back to them in such a way in such a form that the other person recognizes the experience as their own – on a good day that’s how it works – that’s the aha moment – that’s what I was going through – it’s sometimes it could be the very words but often it’s not – often it’s I’ve got inside the movie of your life for a little while – now each of these [four moments of empathy] breaks down in an interesting way and we’re going to therefore look at the breakdown – so this summarizes something interesting and which I think I do want to say it’s always useful to know the order in which one has one slides but basically this is the matter of so we’re gonna, you know, this [talk] is front end loaded – I acknowledge this presentation is somewhat front and loaded because there are several important ideas I want to get into the space and on the table so that we can mix it up about it – but basically so this is the compassion fatigue the burn out moment – heavens knows, occupational hazards – professional challenges – if I may say so – here’s the guidance – this may be for the easier said than done but nevertheless it must both be said and done – and insofar as humanly possible: if I’m interacting with somebody who is suffering, it is highly probable that I am going to suffer – the recommendation, the guidance is, that I have a vicarious experience of that suffering – if I am suffering in such a way that I am in breakdown or upset, [then] I’m doing it wrong
That’s the easier said than done – if I’m overwhelmed by the suffering – as strange as it may say sound to say: I should suffer but not too much – and so this points to the matter of a granularity – to the receptivity – there’s a filter there – right – I mean this all hypothetical – interesting to engage – nevertheless I may want to make the filter more granular and do things to take a little distance so it is not an on/off switch – the takeaway here – not an on/off switch – more like a rheostat – more like a dimmer on a light switch and this is where training and practice make the difference – so I mean we may or may not come back to that – but I want that [statement] in the space so that we can work with it as we get to these examples we’re going to look at – so am I going in the right direction here […] I see we’re just on time –
we look at three or four examples – here I may cut this short because I want to say a little bit more about the training aspect but we’re going to look at Thomas Mass – Thomas Mann is a storyteller – this story got told on or about the year 1900 – it’s about a family the name of Buddenbrooks – they’re a business family – right – and the context is Thomas Buddenbrooks – so here’s the inside skinny – here’s the Birdseye low down on this Buddenbrooks caper – Thomas Buddenbrooks is an artistic type – he’s very artistic – and his father passes away in an untimely way and he – Thomas – goes into the family business to pay the bills – you know, one can understand why one would do this – he gives up his artistic career – his artistic aspirations – and instead of pursuing an artistic career, he marries one – her name is Gerda – she’s an artistic type – we’ll see a picture of her later – […] – she’s playing the violin – she’s a virtuoso violinist – playing passionate virtuoso violin duos with her talented father – it’s so great to have a great relationship […] it’s a very good thing and they have a son – Johann – Hanno, for short – he’s an artistic type – he’s portrayed by Mann as being on sickly – I mean, he’s got bad teeth – this is going to be an issue because this is 1900 – you know dental science – oh my god this has to be interesting –
LA: [ …] some people are already squirming in their seats – it’s working – the mirror neurons are going off even if they don’t exist – this might be a good point to digress – the myth of mirror neurons – professor – C[Jean] Decety – he’s got the MRI machine down at Gates Blake – he recommended this book by Gregory Hitchcock- there’s an underlying neurological mechanism, ladies and gentlemen – it does [or doesn’t] have to be mirror neurons – how about Association? – have you considered a good old-fashioned association? – there’s some implementation mechanism – it’s highly interesting and controversial – I’ll keep the book handy – it’s a scholarly academic debunking […] but what isn’t debunked is our physiological relatedness – even if they [mirror neurons] don’t exist, we’re physiologically related – that’s interesting so and not in the way you might have thought – okay – so anyway you know the dentist – we’re gonna have a trip to the dentist here thanks to Thomas Mass and I’m actually going to read it to you – the paragraph long quotation – so Hanno has bad teeth – in Mann bad teeth are a sign of artistic sensibility – in the case of Hanno he’s kind of sickly – kind of small – he gets bullied by the straggling Nordic types down at school – you know they push him around – it’s not a pretty picture – and his father becomes [a book camp dad] [the father, Thomas] he’s kind of badly compensated – I would say and he’s this hail-fellow-well-met – my son – give me your mathematical multiplication tables – and Hanno knows his tables – he just can’t perform – he breaks down – it’s pathetic – you know but he’s like seven years old – wa, was [crying sounds] – buck up my son – Thomas is boot camp dad and it’s not working – okay – so meanwhile there’s a bit of orality – you know, we can do the oral symbolism – Hanno needs to vigorously suck on the nipple of life and he’s really struggling to engage
[Meanwhile] – off to the dentist doctor – the dentist is already upon dr. brecht – a pun – it’s broken – so I’m gonna read you this slowly –
‘The bad thing about Dr. Brecht was he was nervous and dreaded the tortures he was obliged to inflict – we must proceed to extraction – he would say growing pale – Hanno himself was in a pale cold sweat with staring eyes incapable of protesting or running away – in short, in much the same condition as a condemned criminal – he saw dr brecht’s sleeve and the forceps bending over him and noticed that little beads were standing out on his bald brow and that his mouth was twisted – when it was all over and Hanno, pale and trembling, spat blood into the blue basin at his side dr brecht had to sit down and wipe his forehead and take a drink of water”
LA: So what’s going on here is a breakdown – this is a breakdown in dr. Brecht’s empathic receptivity – he’s overly empathic – one might argue – compare and contrast – the description itself gives us access to the phenomenon – right – both both are sweating – brecht’s mouth is twisted – interesting, the mirror neurons are going off – [brecht’s] his mouth is twisted [so the mirror neurons are going off] – so what’s the recommendation? this is the time for a bad joke – right – he should have gone into ophthalmology – forgive me – okay so back that one out – okay pause for laugh – but anyway it’s a serious insignificant group here – so here’s the breakdown and so what’s the recommendation? – given that empathic receptivity is breaking down on the part of dr. brecht […] – to get some distance from the tortures he inflates – given what is 1900 Dental Science – oh my god – it’s hard to think right and so he has to increase the granularity of the filter – easier said than done but practice practice practice practice what does that look like because he’s providing a useful service – […] I mean, it’s like it’s misery – there’s all kinds of mystery – okay – so you know I pause for breath at this at this point – I would ever take questions even at this point about the example – you know it’s not like this is a quiz and I don’t you know you’re eager for me to move along but don’t be shy raise your hand – okay, so we will move to the next example and that if you think of anything we can circle back around – so remember the set up – Thomas Buddenbrooks gives up his artistic career and he marries someone who is very artistic – Gerda – and she is artistic and she has to move and locate because the Buddenbrookss live in a different town than her father – so she’s no longer playing violin duo’s with her father – she’s got nobody to play with – one might say – so she meets this lieutenant who happens to be a talented violinist in addition to his military aspirations – so they’re upstairs playing passionate violin duo’s and Thomas’s office is downstairs and he’s listening to the violin music – and that’s not the problem – there’s nothing wrong with that – then the music stops – then there’s silence – there’s more silence – there’s even more silence – Thomas is going crazy – Is he going to become the caricature of a jealous husband? – that would be to throw the guy [lieutenant] out – that would be a scandal – that would indeed be a caricature – right – so he’s wandering around pacing back and forth – so he is pacing back and forth and he runs into Hanno in the hallway next quotation –
“His father did not seem to be listening – he held Hannes free hand and played with it absently, consciously fingering the slim fingers and then Hanno heard something that had nothing to do with the lesson at all – his father’s voice in a tone he had never heard before – low distressed almost imploring – Hanno, the lieutenant has been more than two hours with Mama – little Hanno opened wide his golden brown eyes at the sound and they looked as never before clear large and loving straight into his father’s face with his red and eyelids under the light brows its white puffy cheeks and long stiff moustaches – God knows how much he understood – but one thing they both felt in the long second when their eyes met – all constrained coldness in this understanding melted away – Hanno might fail his father in all that demanded vitality energy and strength but where fear and suffering were in question, there they were as one empathic understanding –
Hanno [saw] something that he had not previously perceived – this father was boot camp dad – multiplication tables right – the time goes by – Oh God now he sees – so what’s the word? vulnerability – that’s one possible description – this bootcamp dad is vulnerable – he’s suffering- Hanno does not get it – what does it mean – playing violin duos and then silence -Hanno’s seven or eight years old – right? – so their eyes meet – that is the moment of empathic receptivity embedded in empathic understanding – the father who was so inaccessible in his hail-fellow-well-met and boot camp-style cross-examination of Hanno about his lessons becomes vulnerable and accessible in his suffering – Hanno gets it – his father’s suffering is a possibility – the possibility of his humanity – they share a human moment – the possibility of relatedness emerges in which both are human beings and an emotional connection with one another – this had not been available to Hanno before – for whom his father was this strong demanding taskmaster – now he sees his father’s vulnerability and it humanizes both of them – this is also an example of empathic understanding that works to an extent but ultimately the father remains [in] the role and the story goes along […] What you want to get here is just a picture of the lieutenant and Gerda – they are practicing the violin – she’s giving a master class in practicing the violin – and so let’s do a reality check here – I want to leave both enough time for questions and answers and say something about a little bit more about training
So I’m going to fast-forward through interpretation – if you get the deck you can get some detail and move on to the Glass Menagerie [by] Tennessee Williams who is a formidable psychologist – so the story in brief: Amanda is the mom – Laura is the frail, fragile keeper of The Glass Menagerie – she lives in the back room – she is the daughter – she has a brother, Tom, who has a friend, Jim – Amanda, the mother, had many gentleman callers in her youth – she was popular – we could do with the song from Wicked [the broadway play] at this point but perhaps we won’t – we can we splice that in later – but as she was popular – now she’s fading – the bloom is off the rose – off the flower in the years nineteen fifties – and she so badly wants a date for Laura – to get a date – she wants her to have a gentleman caller caller so she pressures her son, Laura’s brother, Tom, to bring somebody from down at the factory and finally Tom invites Jim, his friend – there’s other information asymmetries in the story – Jim’s already engaged – get ready – you don’t necessarily know that at this point [in the story] but look is to follow along so the invitation is accepted – at last a gentleman caller! – the problem is Jim thinks it’s just a casual dinner with his friend Tom but in fact he then meets Laura who know Jim from grammar school – they went to grammar school together! – it’s small world and Jim sees her and and he says two words: blue roses – blue roses – and Laura is taken aback – she had many childhood illnesses including pleurisy – fluorosis – and when the teacher this was the day when the teacher would say why you weren’t in school well she’s got fluorosis or pleurisy – nobody knew what that meant anyway but Jim hears that as “blue roses” so here’s the part we’ll cut to the chase – Laura also has another childhood disease which leaves one of her legs slightly shorter than the other – polio- and as she walks down the aisle her experience of herself as that she’s making this enormous clomp clomp thumb clomp clomp as she walks down the aisle that everybody must know about it –
of course Jim didn’t even perceive it [it is so soft] and so we have here an example of what amounts to empathic responsiveness – he [Jim] gives her back his experience of who she is for him – for Jim, Laura is “blue roses” – something beautiful even if kind of melancholy – she’s got this melancholy aspect to her which makes her all the more attractive of course – […] and whereas she experienced herself as clunk clunk clunk thunk – the asymmetry there is very powerful – it’s very nice – I think Williams is a brilliant psychologist – I mean – and unfortunately – I mean – he’s also pretty depressed himself and it ends badly – nevertheless we’re going to enjoy the moment – the emotional devastation [is powerful art] – okay, so having so you know that’s three out of four examples – now we’re just on time
I’m going to talk and to tell you about an exercise rather than do the exercise – I call this exercise: I can’t hear you because my opinion of what you are saying is so loud – I’m going to be disarmingly with candid – so you know there I am walking down the street – and I am ashamed of myself – the author of three books on empathy – [and i am thinking devaluing thoughts] – how did that person get to be that way – I’m judging and evaluating – there’s these thoughts – what happened to you man? – wherever it comes, from it’s not authentically Who I am – you want to take this and apply it as appropriate and to yourself: there I can’t hear you because the opinion of what you are saying is so loud in my own thinking – so this is an exercise, not how to listen better, but how to expand one’s listening – right – stop and so actually this is where the the [Dilbert] cartoon comes in handy –
[…] there’s an exercise here that this is how to train for empathy – what does it mean to train empathy – remove the obstacles such as cynicism, categorizing people, labeling, pigeon holing, and so on – I’ll read this to you just so some of you are picking up on it – [in the Dilbert cartoon]: now so there’s the pointy headed boss [and he says] “from now on all teams will be formed on the basis of myers-briggs personality test types” “if you do not have a personality, one will be assigned to you by Human Resources [dept]” – okay, laughter at this point, [this] is deeply cynical […] this is what not to do – right? – and then the final [statement of the cartoon] “we need a quiet dumb guy to pair with an extroverted thinker” – well here the cynicism is what gets in the way of empathy – now that is not to say that it is not abroad in the land of the corporation [and it] goes off the rails – so what I invite – what the exercise consists of doing is going inward and realizing that if one goes inward far enough, one encounters the other – so we actually are going to take literally a half a minute and do the exercise –
So I’m going to ask you to be quiet and listen to yourself […] now there may be papers going off so just include that because this is after all a hospital – […] but listen to what is there – okay are you ready – any questions before they do the exercise? – it is it clear what I’m asking you to do ? please say if it’s not clear […] so you’re just gonna listen to whatever is there okay ready set go
[pause for thirty seconds]
Okay – that’s 30 seconds […] now you might have heard something like “what is he talking about?” “where did this guy come from?” “What voice?” “What conversation?” That’s the one – that’s the one [we are talking about]! – it’s not who I authentically am – and [yet] that is a source of empathic understanding -I am in relationship with the other and I’m going to have judgments, opinions, evaluations, philosophical arguments, categorizations, labels and so on – there isn’t anything wrong with those – those thoughts occur – they are inevitable – you can’t – ladies and gentlemen, you can’t stop thinking those – you can’t prevent it – what you want to do is get some distance from it and realize when it’s useful and when it’s less useful and so with that said we’re going to have some time for questions –
The one final thought I leave you with – and it’s a direct consequence of this little exercise – to listen to oneself, when all the labels are removed, when all the categories are removed, when all the philosophical arguments are removed, when all the cynicism, hostility, affectation, even compassion, sadness, fear, guilt, shame – when all these things are removed, [then] empathy consists in being in the presence of another human being
LA: what are your questions?
LA: The lady in the back – I’ll repeat the question – go ahead –
Do you think you can teach empathy?
LA: The short answer is yes […] so I’m going to repeat the answer – I just [asserted] we’re naturally empathic – remove the cynicism, denial, shame, guilt, and empathy naturally shows up – train the trainer now that’s not considered the possibility […] there other tips and techniques – this is the realm of tips and techniques: my reaction to you tells me something about both of us and a lot about myself which I then parlay forward to understand the relationship
[….] The challenge to create a context in which empathy can show up – right that’s not a trivial things – it’s a lot of work – and of course teaching is information transfer – I put information in your bucket – you bring a bucket or a basket and the teacher puts information in it – there’s nothing wrong with that – we need that – […] the world doesn’t work without information and there’s also the other aspects – dimensions – especially to our humanity and what happens in the context of a conversation – so you know there’s some work to be done on creating [possibility] and that’s what I think [why] literature has its uses in creating a context for a conversation that’s why I find it useful other questions? so I mean feel free to challenme
Individuals have been in some tough spots in the trenches for a while and become hardened – I think you use that word and how does one recover from that? – so I would also put on the list compassion fatigue – burnout – this is a significant occupational hazard – I mean – take some time off for self-care – this is the case for self-care – that one has to find some things where one can restore one’s emotional energies if you will – that we have something like emotional energy – and because being burned out – being compassion fatigued – I ain’t doing nobody any good much less myself – right? – so sometimes one has to get some supervision – I mean now leaving aside matters of such as vacation and that is where I find humor which is closely related to empathy – this Dilbert is deeply cynical right? – but –
in both empathy and humor one traverses a boundary – in the case of humor, one can say look at the boss is an idiot and it’s funny – Human Resources says a personality will be assigned to you – it’s hilarious, right? […] it’s the reduction to absurdly right? – so philosophically, it’s a reduction to absurdity – so one can use humor […] so this is the case for one’s own psychotherapy – I mean that the therapist him or herself may usefully encounter at some point in their development something like whatever this thing is – therapy h- aving a conversation with oneself – journaling – it may become a self-sustaining process – I get a lot out of journaling – I mean some people do and some people don’t – the world is not generous in the matter of certain things such as empathy – put it on the list with compassion as well right? – and so one has to find some resources to recharge one’s empathy – oftentimes it’s family – speaking personally, coming up, I experienced the lack of empathy so I actually started writing about it – and that was how I approached it and I kind of symbolically created something for myself […] – one final question…
LA: we are out of time – one final question?
what is the triad that sustains the therapeutic process? Warmth, accessibility, what else?
LA: okay well the concise answer is the Triad is – empathy empathy and empathy and warm and accessible is also useful – on a good day the other individual will show you who she or he is – if I am present without categories, distinctions, labels – on a good day they’ll reveal their soul – on a less good day we will struggle like everyone else – thank you so much
I heard there was some lunch – I don’t know if there is – I heard it was are up on six – I’m gonna go up there and check it out
(C) Lou Agosta, PhD and the Chicago Empathy Project
Radio Empathy is now on the air as a podcast: New episode: A rigorous and critical empathy: Perform a readiness assessment
Empathy is never needed more than when it seems there is no time for it. Empathy is never needed more than when it seems the budget does not allow for it. Empathy is never needed more than when the cynicism and resignation about life, whether in the family or the corporate jungle, are so thick you can’t catch your breath.
Being ready for empathy is like being ready to be born. No one is ready to be born. You just get born. Ready or not, the individual is thrown into the world. No one asked you if you wanted a life. You just got one.
Empathy enables you to have a human existence filled with satisfying, engaging, dynamic, fulfilling relationships instead of living in an empty, depopulated emotional desert.
There is enough empathy to go around. The key to the empathy readiness assessment is realizing enough empathy is available for everyone. Empathy is not a zero sum game. There do not have to be losers versus winners. If you can get your head around the idea that there is enough empathy available in the world—crazy as that idea may seem at first—then you are ready to engage with expanding empathy in your life and the community.

Seems impossible? Let us take a step back. You know how we can feed everyone on the planet, so that there should be no need for people to get sick and die of starvation? Thanks to the “Green Revolution,” high tech seeds, and the economies of scale of agri-business, enough food exists to feed everyone. Yet people are starving. People are starving in the Middle East, Africa, and in parts of the USA. People are starving because of politics in the pejorative sense, breakdowns in social justice, violence, aggression, bullying, cynicism, bias, prejudice, fragmentation of communities, and human badness. There is enough food to feed everyone, but it is badly distributed.
Likewise, with empathy. Enough empathy is available to go around; but it is not evenly distributed. People are living and working in empathy deserts.
Organizational politics in the pejorative sense of the words, attempts to control and dominate, egocentrism and narcissism, out-and-out aggression and greed, stress and burnout, all result in empathy deserts. Empathy gets hoarded, creating empathy deserts locally, even amid an abundant ability to practice empathy.
Create a clearing for success in working on expanding your empathy, contributing to growing empathy in yourself, other individuals, and the community. Perform a readiness assessment for empathy training
Therefore, this guide to bringing forth a rigorous and critical empathy training does not call for “more” empathy, but rather for “expanded” empathy. The difference is subtle. Commenting “We need more empathy here!” implies the individual is unempathic—are you saying I lack empathy!?—and that is an insult, a dignity violation, a narcissistic injury, creating even more conflict and shrinking empathy.
The way we put our words together makes a profound difference. Experience indicates the call for “more empathy” results in a further breakdown of empathy. In contrast, calling for “expanded empathy” makes a difference in getting unstuck from difficult, sticky situations, reestablishing relatedness, de-escalating conflict, interrupting anger or soothing rage, shifting out of upset, and overcoming the challenges of relating in a world that can from time-to-time be decidedly unempathic.
In extreme cases, a person may in fact lack empathy in a medical or legal sense—the serial killer, the psychopath, and persons suffering from mental illnesses, or, more sympathetically, one of the disorders of empathy such as an autism spectrum disorder. However, such persons are exceptions or in an exceptional situation.
In most cases, individuals have a significant empathic ability with which the individual is out of touch. The person lacks self-knowledge, has a blind spot, and does not know himself to be empathic. The person’s empathy is implicit and is waiting to be expanded. Therefore, a rigorous and critical guide calls out for expanded empathy—to leverage the kernel of empathy that already exists in the person’s humanity and develop it, if not into a mountain, at least into a heaping hill of empathy.
One reason that empathy training programs have not worked or have produced disappointing results is that they train the participants in compassion, being nice, conflict resolution, baby and child care, and a number of worthy and admirable skills. This is all well and good, and the use of compassionate methods is making the world a better place in all these situations. So keep it up. There is nothing wrong with reducing conflict, being nice, agreeable, and so on: do not be “unnice.” But paradoxically something is missing—practicing a rigorous and critical empathy.
Now I do not wish to give anyone a bad name, especially anyone who is committed to empathy, compassion, conflict resolution, or making a difference in overcoming human pain and suffering. On the contrary, I acknowledge and honor one and all. The battle against suffering is joined; we are all on the same side; and we want to deploy our resources wisely.
As soon as one announces a commitment (for example): “I am going to expand empathy in my life,” then all the reasons that it is utterly impossible to do so show up. “What are you thinkin’ fella?” Not enough time. Not enough money. Resistance to empathy does not mean that one fails the readiness assessment to expand one’s empathy. It means that one is a human being.
People have blind spots about empathy. People have blind spots, period. Part of the readiness assessment? Those who take the implicit bias test discover they have biases—often several (see Teaching Tolerance 2020). When it comes to doing the work required actually to listen and respond empathically to others, people make exceptions for themselves—and their biases and inauthenticities. No exceptions!
The one question readiness assessment for empathy is: “Am I ready to do what it takes to clean up my inauthenticities in my practice of empathy?” (Key term: clean up.) Even if you are not completely sure what this means, being willing to agree to the statement is enough to get started.
When it comes to a readiness assessment, the “willingness” is easy. Speaking personally, even lazy people can get their heads around willingness; and once a person puts his foot out onto the slippery slope of willingness, well, it is downhill all way. Sliding downhill may have its occasional bumps, and you have to apply the brake at times; but it is a lot easier than climbing up the hill.
Look it, dude. I would be kidding you if I said no effort is required. Effort is required to expand your empathy. It is going to take something—and, at times, something extra by way of effort. Mostly it requires taking an honest look at oneself. That is not trivial. It may be confronting. But if you are getting vicariously traumatized trying to be empathic, then you are doing it wrong. Throttle back. Take a break.
Being willing to clean up one’s authenticities is precisely the empathy lesson. The “gotcha” is that the inauthenticities in one’s life are not limited just to empathy. However, empathy leads the way. The readiness for a rigorous and critical empathy requires, well, rigor and a willingness to be self-critical. The readiness for empathy requires doing the work required to create a clearing for empathic success, a clearing of integrity and authenticity.
(c) Lou Agosta, PhD and the Chicago Empathy Project
Review: The Empathy Diaries: A Memoir by Sherry Turkle
The short review: the title, The Empathy Diaries: A Memoir (Sherry Turkle New York: Penguin Press, 2021, 357 pp.) reveals that empathy lives, comes forth, in empathy’s breakdowns and failings. Empathy often emerges in clarifying a lack of empathy. This work might have been entitled, less elegantly, “The Lack of Empathy Diaries.” I found the book to be compellingly written, even a page-turner at times, highly recommended. But, caution, this is not a “soft ball” review.”
Do not misunderstand me. Sherry Turkle’s mom (Harriet), Aunt Mildred, grand parents, and the extended Jewish family, growing up between Brooklyn and Rockaway, NY, were empathic enough. They were generous in their genteel poverty. They gloried in flirting with communism and emphasizing, in the USA, it was a federal offense to open anyone else’s mail. Privacy is one of the foundations of empathy – and democracy. Sherry’s folks talked back to the black and white TV, and struggled economically in the lower middle class, getting dressed up for Sabbath on High Holidays and shaking hands with the neighbors on the steps of the synagogue as if they could afford the seats, which they could not, then discretely disappearing.
As Tolstoy famously noted, all happy families are alike. What Tolstoy did not note was that many happy families are also unhappy ones. Figure that one out! Sherry’s answer to Tolstoy is her memoir.
Families have secrets, and one was imposed on the young Sherry. Her mother married Charles Zimmerman, which was her last name as he was the biological father. Within a noticeably short time, mom discovered a compelling reason to divorce Charles. The revelation of his “experiments” on the young Sherry form a suspenseful core to the narrative, about which more shortly.
Mom gets rid of Charles and within about another year marries Milton Turkle, which becomes Sherry’s name at home and the name preferred by her Mom for purposes of forming a family. There’s some weirdness with this guy, too, which eventually emerges; but he does have a penis and a younger brother and sister show up apace.
In our own age of blended families, trial marriages, and common divorce, many readers are, like, “What’s the issue?” The issues is that in the late 1950s and early 1960s, even as the sexual revolution and first feminist wave were exploding on the scene, in many communities, divorce was stigmatizing. Key term: stigma. Don’t talk about it. It is your dark secret.
The rule for Sherry of tender age was “you are really a Turkle at home and at the local deli; but at school you are a Zimmerman.” Once again, while that may be a concern, what’s the big deal? The issue is: Sherry, you are not allowed to talk about it. It is a secret. Magical thinking thrives. To young Sherry’s mind, she is wondering if it comes out will she perhaps no longer be a part of the family – abandoned, expelled, exiled. Even the siblings do not find out about the “name of the father” (a Lacanian allusion) until adulthood. A well kept secret indeed. Your books from school, Sherry, which have “Zimmerman” written in them, must be kept in a special locked cupboard.
How shall I put it delicately? Such grown up values and personal politics – and craziness – could get a kid of tender age off her game. This could get one confused or even a tad neurotic oneself. The details of how all these dynamics get worked out make for a page turner.
Fast forward. Sherry finds a way to escape from this craziness through education. Sherry is smart. Very smart. Her traditionally inclined elders tell her, “Read!” They won’t let her do chores. “Read!” Reading is a practice that expands one’s empathy. This being the early 1960s, her folks make sure she does not learn how to type. No way she is going to the typing pool to become some professors typist. She is going to be the professor! This, too, is the kind of empathy on the part of her family unit, who recognized who she was, even amidst the impingements and perpetrations.
Speaking personally, I felt a special kinship with this young person, because something similar happened to me. I escaped from a difficult family situation through education, though all the details are different – and I had to do a bunch of chores, too!
The path is winding and labyrinthine; but that’s what happened. Sherry gets a good scholarship to Radcliffe (women were not yet allowed to register at Harvard). She meets and is mentored by celebrity sociologist David Reisman (The Lonely Crowd) and other less famous but equally inspiring teachers.
She gets a grant to undertake a social psychological inquiry into the community of French psychoanalysis, an ethnographic study not of an indigenous tribe in Borneo but a kind of tribe nonetheless in the vicinity of Paris, France.
The notorious “bad boy” Jacque Lacan is disrupting all matters psychoanalytic. His innovations consist in fomenting rebellion in psychoanalytic thinking and in the community. “The name of the father” (Lacan’s idea about Oedipus) resonates with Turkle personally.
Lacan speaks truth to [psychoanalytic] power, resulting in one schism after another in the structure of psychoanalytic institutes and societies. Turkle intellectually dances around the hypocrisy, hidden in plain view, but ultimately calls it out: challenging authority is encouraged as long as the challenge is not directed at the charismatic leader, Lacan, himself. This is happening shortly after the students and workers form alliance in Paris May 1968, disrupting the values and authority of traditional bourgeois society. A Rashomon story indeed. Turkle’s working knowledge of the French language makes rapid advances.
Turkle, whose own psychoanalysis is performed by more conventional American analysts in the vicinity of Boston (see the book for further details), is befriended by Lacan. This is because Lacan wants her to write nice things about him. He is didactic, non enigmatic amid his enigmatic ciphers. Jaques is nice to her. I am telling you – you can’t make this stuff up. Turkle is perhaps the only – how shall I put it delicately – attractive woman academic that he does not try to seduce. Lacan “gets it” – even amid his own flawed empathy – you don’t mess with this one. Yet Lacan’s trip to Boston – Harvard and MIT – ends in disaster. This has nothing – okay, little – to do with Turkle – though her colleague are snarky. The reason? Simple: Lacan can’t stop being Lacan.
Turkle’s long and deep history of having to live with the “Zimmerman / Turkle” name of the father lie, hidden in plain view, leaves Turkle vulnerable in matters of the heart. She meets and is swept off her feet by Seymour Papert, named-chair professor at MIT, an innovator in computing technology and child psychology, the collaborator with Marvin Minsky, and author of Mindstorms: Children, Computers and Powerful Ideas.
Seymour ends up being easy to dislike in spite of his authentic personal charm, near manic enthusiasm, interestingness, and cognitive pyrotechnics. Warning signs include the surprising ways Sherry have to find out about his grown up daughter and second wife, who is actually the first one. Sherry is vulnerable to being lied to. The final straw is Seymour’s cohabitating with a woman in Paris over the summer, by this time married to Sherry. Game over; likewise, the marriage. To everyones credit, they remain friends.
Sherry’s academic career features penetrating and innovative inquiries into how smart phone, networked devices, and screens – especially screens – affect our attention and conversations. The research methods are powerful: she talks to people, notes what they say, and tries to understand their relationships with one another and with evocative objects, the latter not exactly Winnicott’s transitional objects, but perhaps close enough for purposes of a short review.
The reader can imagine her technology mesmerized colleagues at MIT not being thrilled by her critique of the less than humanizing aspects of all these interruptions, eruptions, and corruptions of and to our attention and ability to be fully present with other human beings.
After a struggle, finding a diplomatic way of speaking truth to power, Turkle gets her tenured professorship, reversing an initial denial (something that rarely happens). The denouement is complete. The finalè is at hand.
Sherry hires a private detective and reestablishes contact with her biological father, Charles. His “experiments” on Sherry that caused her mother to end the marriage, indeed flee from it, turn out to be an extreme version of the “blank face” attachment exercises pioneered by Mary Main, Mary Ainsworth and colleagues, based on John Bowlby’s attachment theory. The key word here is: extreme. I speculate that Charles was apparently also influenced by Harry Harlow’s “love studies” with rhesus monkeys, subjecting them to extreme maternal deprivation (and this is not in Turkle). It didn’t do the monkeys a lot of good, taking down their capacity to love, attachment, much less the ability to be empathic (a term noticeably missing from Harlow), leaving them, austic like emotional hulks, preferring clinging to surrogate cloth mothers to food. Not pretty. In short, Sherry’s mother comes home unexpectedly to find Sherry (of tender age) crying her eyes out in distress, all alone, with Charles in the next room. Charles offers mom co-authorship of the article to be published, confirming that he really doesn’t get it. Game over; likewise, the marriage.
On a personal note, I was engaged by Turkle’s account of her time at the University of Chicago. Scene change. She is sitting there in lecture room Social Science 122, which I myself frequented. Bruno Bettelheim comes in, puts a straight back chair in the middle of the low stage, and delivers a stimulating lecture without notes, debating controversial questions with students who were practicing speaking truth to power. It is a tad like batting practice – the student throws a fast ball, the Professor gives it a good whack. Whether the reply was a home run or a foul ball continues to be debated. I was in the same lecture, same Professor B, about two years later. Likewise with Professors Victor Turner, David Grene, and Saul Bellow of the Committee on Social Thought. My own mentors were Paul Ricoeur (Philosophy and Divinity) and Stephen Toulmin, who joined the Committee and Philosophy shortly after Turkle returned to MIT.
Full discourse: my dissertation on Empathy and Interpretation was in the philosophy department, but most of my friends were studying with the Committee, who organized the best parties. I never took Bellow’s class on the novel – my loss – because it was credibly reported that he said it rotted his mind to read student term papers; and I took that to mean he did not read them. But perhaps he actually read them, making the sacrifice. We will never know for certain. One thing we do know for sure is that empathy is no rumor in the work of Sherry Turkle. Empathy lives in her contribution.
(c) Lou Agosta, PhD, and the Chicago Empathy Project
Empathy and Freud: Lost in translation
Freud is explicit about his commitment to empathy. He writes and publishes the following:
It is certainly possible to forfeit this first success [in therapy] if one takes up any standpoint other than one of empathy such as moralizing (“Further recommendations: On beginning the treatment.” Standard Edition of the Complete Psychological Works of Sigmund Freud, Volume 12: 121-144. : 140).
Unfortunately no one knows that Freud wrote that, because it is literally lost in translation. In translating “empathy [“Einfühlung”] from the original German, Alix Strachey writes to James Strachey: “In any case, it’s a vile word [“empathy”], elephantine, for a subtle process.” The words “sympathetic understanding” were chosen as the translation in this case. The rest, as they say, is history; except that it is like Russian history when Stalin had Trotsky’s photos literally cut out of the history books of the Russian Revolution. Talk about repression!
[Note: This post is an excerpt from Chapter Four of my book A Rumor of Empathy: Rewriting Empathy (Palgrave Publishing): to buy the book or have your local library order a copy go here: get A Rumor of Empathy: Rewriting Empathy [https://tinyurl.com/y24ps876]]
Freud’s method was an empathic one, and the dispute, if any, is not that Freud did not use or value empathy. He did. Freud applies empathy in his clinical practice, even when he does not use the word “Einfühlung.” Freud balances his commitment to empathic methods even in the face of the boundary issues of C. G. Jung and S. Ferenczi with their women patients, where Freud took the moral high ground, counseled the need to be dispassionate and “like a surgeon” in neutrality, anonymity, and (above all) abstinence. However, that may all be well and good in practice, but how does that work in theory?
In theory Freud limited his explicit mentions of “empathy.” The reason is Freud’s definition of “introspection.” Introspection is distinct from empathy, but closely connected to it. One dominant modern definition of empathy is “vicarious introspection” (Kohut 1959), where introspection is the royal road to empathy. Introspection is an anchor, making available the spontaneously arising vicarious feelings that are further processed by empathic understanding and interpretation into an empathic response. Yet Freud did not make such a distinction. Rather Freud defines “introspection” in terms of the self-observation of the conscience (one aspect of the superego), that is, as a form of self-criticism and censorship.
In this quotation, empathy is distinguished from “moralizing.” This is a casual reference but a potentially revealing one. By “moralizing” one understands Freud to mean the use of “approval” or “blame” as means of influencing the course of treatment. The exclusion of an ethics of empathy does not rule out the use of empathy for recognition of the humanity of the other person. In this sense, empathy implies a respect for the autonomy of the other which is inconsistent with any attempts to manipulate him by means of approbation and punishment. It is important to keep open a space for the ethical implications of empathy without indulging in “moralizing” in the narrow sense.
As noted,, this is also the text in which “Einfühlung[empathy]” is mistranslated by Strachey as “sympathetic understanding,” thus further obscuring the critical role that it takes in Freud’s practice. Contrary to Strachey, Freud takes significant effort to distinguish “empathy” from “sympathy.”
The effort to distinguish “empathy” from “sympathy” continues in Freud’s “Preface to Aichhorn’s Wayward Youth”(1925: 273). Sadly, so does the mistranslation. Freud acknowledges the contribution of August Aichhorn in working with troubled adolescents: “His [Aichhorn’s] attitude to his charges sprang from a warm sympathy with the fate of those unfortunates and was correctly guided by an intuitive perception [“intuitive Einfühlung” = “intuitive empathy”] of their mental needs.”
The use of “intuition” here is not the over-intellectualization about which Kohut cautioned (e.g., Kohut The Analysis of the Self: 302-305), but rather the recommendation to be guided in relating to the troubled adolescent by one’s perceptive personal reaction, a skill in which Aichhorn excelled.
Freud typically finds a model taken from everyday life for pathological phenomena. Examples include: mourning (normal) and melancholy (depression); dreams (normal) and hallucinatory psychosis (waking dream); religious practices (normal) and obsessional rituals (pathological); love (normal) and hypnosis (abnormal): all present parallels between the everyday and the pathological. Thus, Freud notes the continuum between the pathological state of paranoia and the self-observations of the scrupulously moral conscience:
. . . The self-criticism of conscience is identical with, and based upon, self-observation. That activity of mind, which took over the function of conscience, has also enlisted itself in the service of introspection, which, in turn, furnishes philosophy with the material for its intellectual operations. This must have something to do with the characteristic tendency of paranoiacs to form speculative systems.
It will certainly be of importance to us if we can see in other fields evidence of the activity of this critically watching faculty, which becomes heightened into conscience and philosophic introspection (Recommendations for physicians beginning psychoanalysis, 1914: 96-97).
This definition of introspection as critical self-observation is far from the kind of introspection actually practiced by both the analyst and analysand. The latter’s free associations cannot be generated so long as the conscience is actively censoring one’s thoughts and discourse. The analyst does not deliberately concentrate his attention or listen for anything specific in the analysand’s free associations.
The analyst maintains an attitude of evenly-hovering attention, in which his tendency to “moralize”—approve or blame—is suspended. In this way, introspection on the part of the analyst can disclose vicarious feelings as well as memories analogous to those told by the analysand. In both cases, we have a kind of introspection without inspection (to coin a phrase), which conditions the arousal of empathic receptivity towards the latent content of the analysand’s unstudied associations.

Rehabilitating introspection without inspection is based on an account of empathic receptivity. In so far as empathy is a kind of vicarious introspection, Freud’s ambivalence towards introspection constrains his use of empathy. Having a limited conception of the uses of introspection as “moralistic,” critical self-observation in philosophy constrained Freud’s explicitly using empathy as a means of empathic receptivity towards the introspective accounts of the analysand and the analyst’s own vicarious feelings thus aroused.
In short, Freud’s methods and listening were highly empathic, and if one’s experience today is otherwise, it is only because something has been lost in translation – empathy.
“Okay, I’ve read enough; I want further details”: to buy the book or have your local library order a copy of this book or another of Lou’s empathy books go here: get A Rumor of Empathy: Rewriting Empathy [https://tinyurl.com/y24ps876]

Freud’s empathy: Freud depicted in front of the empathy control panel: Empathy is a dial, not an on-off switch
(c) Lou Agosta, PhD and the Chicago Empathy Project
A Lazy Person’s Guide to Empathy, the book, now available: Expand empathy in the individual and community today!
Empathy: A Lazy Person’s Guide is a light-hearted look at a significant and engaging matter: how to expand empathy in the individual and the community – and do so without working too hard. The Guide includes twenty eight illustrations by the celebrated artist Alex Zonis. So if you get tired of reading, look at the pictures! Practically an art book, get a summary in line below and order the book here and now by clicking here: Empathy: A Lazy Person’s Guide.
Given current events (Q2 2020), go straight to the section on applying empathy to soothe anger and rage – and setting empathic limits to drive out bullying, prejudice, and bad behavior. In addition –
A lazy person’s guide to empathy guides you in –
- Performing a readiness assessement for empathy

- Cleaning up your messes one relationship at a time.
- Defining empathy as a multi-dimensional process.
- Empathy in the age of coronavirus – don’t miss it!
- Overcoming the Big Four empathy breakdowns.
- Applying introspection as the royal road to empathy.
- Identifying natural empaths who don’t get enough empathy – and getting them [oneself] the empathy one needs.
- The one-minute empathy training. [No kidding!]
- Compassion fatigue: A radical proposal to overcome it.
- Listening: Hearing what the other person is saying versus your opinion of what she is saying.
- Distinguishing what happened versus what you made it mean.
- Applying empathy to sooth anger and rage.
- Good fences (not walls!) make good neighbors: About boundaries.
- How and why empathy is good for one’s well-being.
- Empathy and humor.Empathy, capitalist tool.
- Empathy: A method of data gathering.
- Empathy: A dial, not an “on-off” switch.
- Assessing your therapist,.
- Applying empathy in every encounter with the other person – and just being with other people without anything else added.
- Empathy as the new love – so what was the old love?
The lazy person’s guide to empathy offers a bold idea: empathy is not an “off-off” switch, but a dial or tuner. The person going through the day on “automatic pilot” needs to “tune up” or “dial up” her or his empathy to expand relatedness and communication with other people and in the community.
Practicing empathy includes finding your sense of balance, especially in relating to people. In a telling analogy, you cannot get a sense of balance in learning to ride a bike simply by reading the owner’s manual. Yes, strength is required, but if you get too tense, then you apply too much force in the wrong direction and you lose your balance. You have to keep a “light touch.” You cannot force an outcome. If you are one of those individuals who seem always to be trying harder when it comes to empathy, throttle back. Hit the pause button. Take a break.
Empathy is about balance: emotional balance, interpersonal balance and community balance. Empathy training is all about practicing balance: You have to strive in a process of trail and error and try again to find the right balance. So “lazy person’s guide” is really trying to say “laid back person’s guide.” The “laziness” is not lack of energy, but well-regulated, focused energy, applied in balanced doses. The risk is that some people – and you know who you are – will actually get stressed out trying to be lazy. Cut that out! Just let it be.
The natural empath – or persons experiencing compassion fatigue – may usefully “tune down” their empathy. But how does one do that?
The short answer is, “set firm boundaries.” Good fences (fences, not walls!) make good neighbors; but there is gate in the fence over which is inscribed the welcoming word “Empathy.”
The longer answer is: The training and guidance provided by this book – as well as the tips and techniques along the way – are precisely methods for adjusting empathy without turning it off and becoming hard-hearted or going overboard and melting down into an ineffective, emotional puddle.
Empathy can break down, misfire, go off the rails in so many ways. Only after empathy breakdowns and misfirings of empathy have been worked out and ruled out – emotional contagion, conformity, projection, superficial agreement in words getting lost in translation – only then does the empathy “have legs”. Find out how to overcome the most common empathy breakdowns and break through to expanded empathy – and enriched humanity – in satisfying, fulfilling relationships in empathy.
Okay – I have read enough – I would like to order the book: click here: Empathy: A Lazy Person’s Guide.
(c) Lou Agosta, PhD and the Chicago Empathy Project